Autor :Terroba, Hernán1, Sánchez Hinestroza, SofĂa1, González, Alejandra1, Alzola, Rodrigo2, Segovia, Jaime1, Fielli, Mariano1
1Pulmonology Service, Hospital Nacional Profesor Alejandro Posadas, Buenos Aires, Argentina.
2Infectology Service. Hospital Nacional Profesor Alejandro Posadas, Buenos Aires, Argentina.
https://doi.org/10.56538/ramr.NVKD9714
Correspondencia : Hernán Terroba. E-mail: hterroba@gmail.com
ABSTRACT
Diffuse infiltrative
lymphocytosis syndrome (DILS) occurs in association with HIV infecÂtion; it
requires that diagnostic criteria are met and other infectious and autoimmune
diseases are discarded. We present the case of a 47-year-old woman who
consulted for bilateral parotid swelling, sicca
syndrome, cough and impregnation syndrome; chest tomography showed patchy
bilateral ground glass infiltrate. The patient was diagnosed with HIV, and fiberoptic bronchoscopy with bronchoalveolar
lavage (BAL) was performed, without pathogen growth. It is interpreted as
lymphoid interstitial pneumonia associated with DILS. Antiretroviral therapy
was started, with good evolution and disappearance of symptoms and pulmonary
infiltrates.
Key words: Diffuse infiltrative lymphocytosis syndrome (DILS), Human
immunodeficiency virus, Interstitial pneumonia
RESUMEN
El síndrome de linfocitosis infiltrativa
difusa se produce en asociación con la infección por virus de la
inmunodeficiencia humana; requiere cumplir con los criterios
diagnósticos y descartar otras patologías infecciosas y
autoinmunes. Se presenta el caso de una mujer de 47 años que
consultó por edema parotídeo bilateral, síndrome sicca, tos y síndrome de impregnación. Se
observó en la tomografía de tórax infiltrado en “vidrio
esmerilado”, parcheado y bilateral. Se realizó diagnóstico de
virus de la inmunodeficiencia humana positivo y fibrobroncoscopia
con lavado broncoalveolar sin desarrollo de
patógenos. Se interpreta como neumonía intersticial linfoidea
asociada a síndrome de linfocitosis infiltrativa
difusa. Se inició terapia antirretroviral con buena evolución y
desaparición de los síntomas y de los infiltrados pulmonares.
Síndrome de linfocitosis infiltrativa
difusa, Virus de la inmunodeficiencia humana, Neumonía intersticial
linfoidea
Received: 6/17/2022
Accepted: 8/18/2022
INTRODUCTION
DILS is associated with the human
immunodefiÂciency virus (VIH), characterized by dry eyes and dry mouth (sicca syndrome), lymphadenopathies, bilateral parotitis
and extra-glandular involveÂment. It was initially identified in 1985 as lymph
node hyperplasia and parotid gland enlargement in HIV patients.1 Then, in 1989, this complex
was called DILS, and its association with host factors was defined as antigens
of the major histocompatÂibility complex and increased frequency of HLA-DR5,
thus determining the presence of a genetiÂcally defined immune response to HIV
infection.2 The estimated prevalence is
7.8% in the era before the antiretroviral therapy (ART), which was then reduced
to 1.5% with said treatment.3-4
We present a case of sicca syndrome associÂated with recent diagnosis of HIV
infection with lymphoid interstitial pneumonia (LIP) and DILS.
CASE REPORT
47-year-old
female patient with history of smoking and hypothyroidism. She presented with a six-month history of painless
edema in bilateral parotid region, dry cough, dry mouth and dry eyes, night
sweating, and weight loss (20 kg).
The neck ultrasound
showed enlarged parotid glands of diffuse heterogeneous aspect. Lab results:
blood count without eosinophilia; PCR: 4.7 mg/d, positive serology for HIV,
with CD4+ 253 mm3 /CD8+ 1159 mm3 values, viral load of 186.340
copies/ml, negative collagenogram, normal IgE values, normal proteinogram.
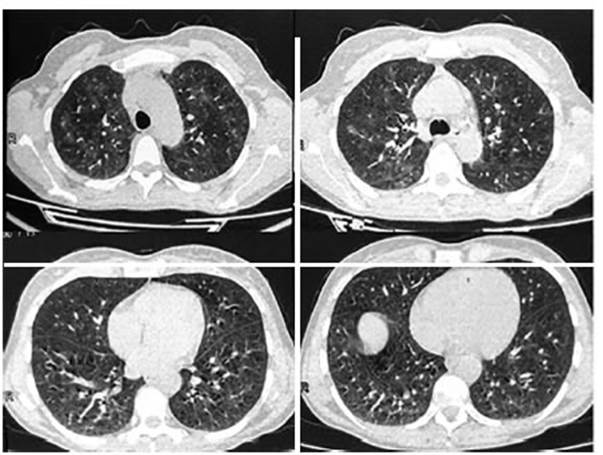
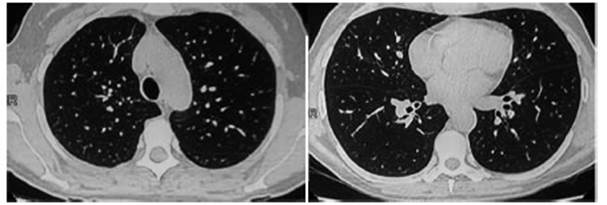
The chest CT showed
patchy ground glass infiltrate with bilateral involvement and diffuse
distribution; subtle presence of predominantly peripheral reticulum and some
isolated cysts (Fig. 1). A fiberoptic bronchoscopy
with BAL was performed, evidencing 28% lymphocytosis without microbiological
isolates and negative PCR for Pneumocystii jirovecci. The patient refused to undergo a biopsy of
the parotid due to the possible complications of this procedure. The symptoms
were interpreted as lymphoid interstitial pneumonia related to DILS, so the
patient began antireÂtroviral therapy.2 Currently without respiratory symptoms, parotid glands
reduced in size, undetectable viral load with increased CD4/CD8 ratio.
DISCUSSION
Sicca syndrome is one of the rheumatologic manifesÂtations
that can be present in patients with HIV.5,6 The DILS is defined as an
entity associated with HIV and is characterized by the Sicca
syndrome, adÂenopathies, bilateral parotitis and extra-glandular involvement, which is based
on tissue destruction due to CD8+lymphocyte infiltration. At the peÂripheral
blood level, we observe lymphocytosis with expansion of CD8+ cells, and a low
CD4/CD8 ratio. Clinical manifestations secondary to the extra-glandular
visceral involvement depend on the affected organ: nervous system with aseptic
meningitis, polyneuropathy of acute or sub-acute onset, paralysis of the facial
nerve, lymphocytic hepatitis, tubulointerstitial
nephritis, cystitis and gastrointestinal infiltration.7-8
The prevalence of
pulmonary involvement varÂies according to the different series in 33 to 66% of
the cases. The most common clinical and radiologiÂcal presentation is lymphoid
interstitial pneumoÂnia (LIP). The chest CT shows areas of bilateral ground
glass infiltrate, ill-defined centrilobular
nodules, thin-walled cysts, septal thickening and
interlobular reticulations.9
No consensus has been
reached regarding the diagnostic criteria for DILS, and no standards have been
established, either. However, some authors such as Itescu
et al propose the following diagnostic criteria:
1) Positive serology
for HIV.
2) Bilateral swelling
of salivary glands or dry mouth with persistence of signs or symptoms for at
least 6 months.
3) Histological
confirmation of lymphocytic infilÂtration of the salivary or lacrimal glands
without granulomatous or neoplasic involvement.10
BAL is useful for
discarding an underlying opÂportunistic infection, and typical findings include
an increase in the total white blood count with lymphocytosis and a normal
count in the CD4/ CD8 ratio.
The differential
diagnosis includes the Sjögren syndrome (SS), which has
the same signs as the Sicca syndrome, parotitis, extra-glandular maniÂfestations (mainly
involving the lung, the nervous system and the kidney) and hypergammaglobuÂlinemia.
In the SS, we can observe the presence of autoantibodies: FAN with anti-SSA/Ro,
anti-SSB/ La in SS and organ infiltration by CD4+ lymphoÂcytes, whereas in DILS
there will always be HIV patients and infiltration by CD8+11 lymphocytes. We must also
exclude other “Sjögren-like” synÂdromes
such as IgG4-related disease, chronic hepatitis C and chronic graft-versus-host
disease.
With regard to the
treatment, most authors agree on the administration of ART, also considerÂing
the use of steroids according to the severity of the symptoms.12
In the case presented
herein, the systemic cliniÂcal characteristics and pulmonary radiographic
features, the absence of autoantibodies and favorÂable clinical evolution after
beginning antiretroviÂral therapy allow us to presume a DILS diagnosis, since
the histological confirmation couldn’t be obtained due to patient’s refusal.
CONCLUSION
DILS is a multisystem
syndrome with a currently low prevalence. Interstitial pneumonia can be one
manifestation and must be included in the differential diagnosis.
Conflict of interest
Authors have no
conflict of interest to declare.
REFERENCES
1. Solal-Celigny P, Couderc LJ,
Herman D, et al. Lymphoid interstitial pneumonitis in acquired immunodeficiency
synÂdrome-related complex. Am. Rev Respir Dis. 1985;131:956- 60. https://doi.org/10.1164/arrd.1985.131.6.956
2. Itescu S, Brancato LJ, Winchester
R, et al. A sicca syndrome in HIV infection:
Association with HLA-DR5 and CD8 lymÂphocytosis. Lancet 1989;2:466-8. https://doi.org/10.1016/s0140-6736(89)92085-0
3. Williams FM, Cohen
PR, Jumshyd J, Reveille JD. PrevaÂlence
of the diffuse infiltrative lymphocytosis syndrome among human immunodeficiency
virus type 1-positive outpatients. Arthritis Rheum.
1998;41:863-8. https://doi.org/10.1002/1529-0131(199805)41:5<863::AID-ART13>3.0.CO;2-F
4. Panayiotakopoulos GD, Aroni K, Kyriaki D, et al. Paucity of Sjögren-like
syndrome in a cohort of HIV-1-positive patients in the HAART era. Part II.
Rheumatology (OxÂford) 2003;42:1164-7.
https://doi.org/10.1093/rheumatolÂogy/keg316
5. Yamamoto M, Nakao R, Higuchi Y, et al. sicca
syndrome in patients infected with human immunodeficiency virus-1. Mod Rheumatol. 2002;12:333-7.
https://doi.org/10.3109/s101650200059
6. Meer S. Human
immunodeficiency virus and salivary gland pathology: an update. Oral Surgery, Oral Medicine, Oral Pathology and Oral Radiology.
2019;128:52-9.
https://doi.org/10.1016/j.oooo.2019.01.001
7. Sidahi M, Luque
R, Martínez A, Mañas MD. Síndrome de linfocitosis infiltrativa difusa: otra causa de fracaso renal agudo en
paciente VIH [Diffuse infiltrative
lymphoÂcytosis syndrome: another cause of acute renal failure in the HIV-infected patient]. Enferm Infecc Microbiol
Clin. 2010;28:757-8.
https://doi.org/10.1016/j.eimc.2010.06.004
8. Ghrenassia E, Martis N, Boyer J, Burel-Vandenbos F, MeÂkinian A, Coppo P. The diffuse infiltrative
lymphocytosis syndrome (DILS). A comprehensive review.
J Autoimmun. 2015;59:19-25. https://doi.org/10.1016/j.jaut.2015.01.010
9. Oikonomou A, Prassopoulos P.
Mimics in chest disease: interstitial opacities. Insights
Imaging. 2013;4:9-27. https://doi.org/10.1007/s13244-012-0207-7
10. Itescu S, Winchester R. Diffuse infiltrative lymphocytosis
syndrome: a disorder occurring in human immunodeficienÂcy virus-1 infection
that may present as a sicca syndrome. Rheum Dis Clin North Am. 1992;18:683-97.
11. Ghrenassia E, Roulin L, Aline-Fardin A, et al. The spectrum of chronic CD8+ T-cell
expansions: clinical features in 14 patients. PLoS One. 2014;9(3):e91505. Published 2014 Mar 11.
https://doi.org/10.1371/journal.pone.0091505
12. Nizamuddin I, Koulen P, McArthur
C. Contribution of HIV Infection, AIDS, and Antiretroviral Therapy to Exocrine
Pathogenesis in Salivary and Lacrimal Glands. Int J Mol Sci. 2018;19:2747.
https://doi.org/10.3390/ijms19092747