Autor : Marco Antonio GarcÃa Choque
Bronchoscopy Service, Instituto Nacional de Tórax, La Paz - Bolivia
Correspondencia : E-mail: marcoantoniogar@hotmail.com
Abstract
Mucocutaneous leishmaniasis is relatively frequent in the tropical regions of Bolivia. It coexists with another endemic disease of the region: tuberculosis. Tuberculosis frequently affects the upper airways, too. Leishmaniasis may be confused with tuberculosis, thus, its treatment can be erroneous. We report a case of leishmaniasis whose involvement profle is typical of tuberculosis.
Key words: Mucocutaneous leishmaniasis; Tropical ulcer; Espundia
Introduction
Twenty-one species of Leishmania have been
identified as human pathogens. They are systematically divided into four complexes: Two New World
Leishmania species complexes, the L. mexicana
complex (also containing L. amazonensis) and the
L. brazilensis complex (containing L. panamensis
and L. guyanensis ), and two Old World Leishmania
complexes, the L. principal complex (containing L.
tropica ) and the L. donovani complex (also containing L. infantum, also known as L. chagasi)16, 17.
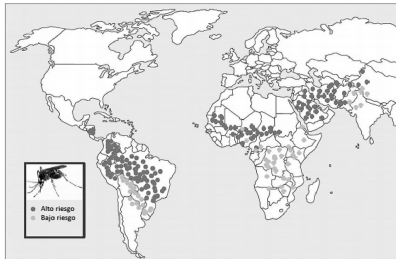
More than 12 million people worldwide are infected with leishmaniasis; 350 million people are
at risk. Leishmaniasis is generally an endemic disease in 98 countries and regions; it is responsible
for a burden of disease of 2.35 million disability-adjusted life years (DALYs), 2.3% of which occur
in the Americas. 75% of all cutaneous leishmaniasis cases are estimated to be concentrated in
10 countries, four of which are in the Americas:
Brazil, Colombia, Peru and Nicaragua. Fifteen
out of 22 species of Leishmania causing disease
in humans have been identified in the Americas,
and 54 different species of vectors are potentially
implicated in its transmission. In the Americas,
an average of 60,000 cases of cutaneous and mucosal leishmaniasis and 4,000 cases of visceral
leishmaniasis are diagnosed every year, with a 7%
mortality rate (Fig. 1).
It is possible to certify that, up to this day,
there are 4 parasitic species of leishmaniasis in
Bolivia: Leishmania (V) braziliensis; Leishmania
(L) amazonensis; Leishmania (L) chagasi and L.
(V) lainsoni. The first species is an agent of mucocutaneous leishmaniasis (MCL); the second one is
an agent of cutaneous Leishmania (CL) and diffuse
cutaneous Leishmania (DCL). These two species
clearly predominate in the national epidemiologic
indices of the disease. The third species is an agent
of visceral leishmaniasis (VL), and the fourth species produces rare cases of cutaneous leishmaniasis (CL). The third and fourth species generate
sporadic clinical cases3, 4.
In Latin America, 90% of mucocutaneous leishmaniasis occurs in Bolivia, Brazil and Peru, appearing as a complication in 5-20% of cutaneous
leishmaniasis cases. It is generally produced by
hematogenous dissemination of the parasite after
a skin lesion, but may also disseminate by lymphatic route or direct extension of facial lesions.
The mucosal involvement may be simultaneous
with the skin lesion, or it may appear months, even
decades after the occurrence of the primary lesion.
The most frequently affected mucosa is the nasal
mucosa, with septum involvement in up to 90% of
the cases. Mucocutaneous leishmaniasis may also
involve the palate, pharynx, larynx and upper lip.
Palate lesions have a polypoid aspect. Laryngeal
involvement consists in the presence of lesions ofa granulomatous aspect infiltrating the mucosa
and vocal cords, which can lead to death from
superinfection or obstruction.
Up to this day, more than 112 species of phlebotomus have been described in Bolivia, 5 of which
are proven vectors of certain type of parasite.
In the Interandean Valley region (Yungas-La
Paz), 2 out of the 17 antropophilic species that
were found have an important role as vectors:
Lutzomyia longipalpis (dominant species in peridomestic settings), as a vector of Leishmania (L)
chagasi, and Lutzomyia nuneztovari anglesi (dominant species in coffee plantations and remnant
vegetation) with a role in the transmission of L.(L)
amazonensis and L. (V) braziliensis9, 10.
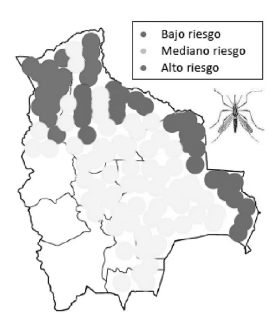
In Bolivia, since ancient times, the disease has
been related to one single population, los Yungas
from La Paz Department. Nowadays, more cases
are being reported among the Yungas “urban” populations (anthropization of the cycle). The new
colonization regions, where important strategic development projects are being organized with mass
population migrations, have spread the disease to
6 Departments (La Paz, Cochabamba, Santa Cruz,
Beni, Pando, Tarija12 (Fig. 2).
The worldwide prevalence of the disease is estimated to be 12 million cases throughout the world,
with an incidence of 2 million new cases per year.
Mucocutaneous leishmaniasis has been first
described in Bolivia by Dr. Manuel Antonio Vaca
Diez in 1,876. It was studied for the first time during the Acre War, when many cases were observedat the Mapiri River and the Colonial Territories.
Elías Sagárnaga (1,904), Adolfo Flores (1,904),
Arturo Ballivian Otero (1,905) and Jaime Mendoza (1,906) used the term ESPUNDIA to identify “tropical ulcers” of any origin. A few years later,
Escomel (1,911) verified the presence of the amastigote parasite in certain patients with “espundia”,
using this term to refer exclusively to American
tegumentary leishmaniasis14-16.
Leishmaniasis is a zoonosis produced by Leishmania (V) braziliensis (Vianna 1,911). It has abroad geographical distribution, from Central
America to the north of Argentina, and is characterized by exacerbated cellular immunity that
can be clinically translated to destructive and
disfiguring mucocutaneous lesions of the oral and
nasopharyngeal regions that appear lately after
the primary ulcers have healed (access point for
the parasite). These lesions show a granuloma
consisting of macrophages and lymphocytes with
very few parasites15.
The following is a case of mucocutaneous leishmaniasis affecting the area that goes from the
upper airway to the tracheal bifurcation.
Clinical Case
Male patient, 50 years old, born in Palca (Lowlands of Bolivia), who worked in a gold mine of a tropical region for 20 years, until 8 years ago. 2 years ago he came to this hospital (Instituto Nacional de Tórax-La Paz- Bolivia) because he had a productive cough and dysphonia. The laryngoscopic examination showed a partially amputated epiglottis and non-valuable vallecules; the glottic area was occupied by nodular lesions of granulomatous aspect. The diagnostic impression was laryngeal tuberculosis and “probable” leishmaniasis. The pathology report showed “specific chronic laryngitis”. The sputum smear test was negative. The patient was referred to the otolaryngology service of another hospital center, where he was finally diagnosed with “tuberculous laryngitis”, taking into account epidemiology, clinical examinations and another laryngoscopy. The patient began anti-tuberculous therapy but suspended it after a month due to gastric intolerance.
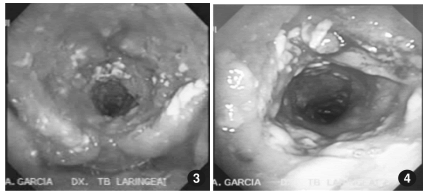
The patient decided not to receive medical care
for a period of two years, after which he came tothis hospital again with chronic mucopurulent
expectoration and dysphonia.
He had never shown any skin lesions. The physical examination showed rhonchus at both lung
bases. Serologic tests for human immunodeficiency
virus (HIV), the venereal disease research laboratory (VDRL) test, the purified protein derivative
(PPD) test, the smear test, the acid-alcohol resistant bacilli (AARB) culture, the bacteriologic
culture and a deep mycosis study of samples taken
from laryngeal lesions and the bronchoalveolar
lavage (BAL) analysis all came back negative. The
chest X-ray showed paracardiac alveolar infiltrate
and two-sided supradiaphragmatic infiltrate.
The patient underwent a fibro-laryngo-tracheobronchoscopy that showed mucosal edema and
multiple ulcers in both nostrils. The pharynx lost
its morphological features and was turned into a
narrow channel with granulomatous lesions, purulent discharge and fibrin stuck to the pharyngeal
walls. The lesions ran from the pharynx to the
trachea in its full extension.
The larynx showed partial amputation of the
epiglottis and granulomatous lesions in its full
extension. Vocal cords could only be identified
with phonation. The subglottis and tracheal lumen showed 25% diameter reduction, with similar
lesions. Lesions of a caseous aspect were observed
next to the carina. The bronchial structure was
preserved, but the primary left bronchus had an
excessive amount of purulent discharge.
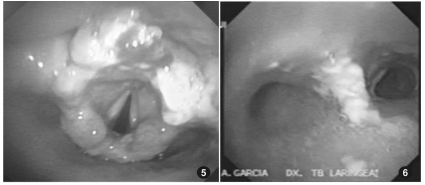
The histopathological report of a new lesion
biopsy showed “non-specific chronic granulomatous inflammatory process.” The smear test of
laryngeal and pharyngeal samples was negative.
Scarification smear and Giemsa stain tests were
negative. Serologic tests: The enzyme-linked immunosorbent assay (ELISA) for antileishmania brazilensis antibodies had POSITIVE results. The
Montenegro intradermoreaction (MIDR) test that
was conducted 48 hours later showed an 8x11 mm
reaction (positive MIDR).
After confirming the immunologic tests and
the epidemiological record, it was decided to start
treatment with meglumine antimoniate (Glucan-
time®) at a given dose of 20 mg/kg daily for 30 days.
The patient showed improvement a week after
initiation. Clinical examinations performed at the
completion of treatment confirmed the favorable
evolution of the symptoms, with an improvement
of voice and respiratory distress. A new endoscopic
control study conducted after 6 months showed
that the epiglottis was still decapitated but less
afflicted with edema and the vocal cords could
be seen with preserved mobility. Tracheal and
bronchial walls did not have lesions of a nodular
aspect, but still showed pathological discharge19-25.
Discussion
Leishmaniasis generally starts with the appearance of an ulcerated skin lesion at the parasite
inoculation site and is less frequent with mucosal
lesions caused by hematogenous dissemination.
This case describes a patient from the Lowlands,
an area endemic for tuberculosis, who worked at
the Tropic, an area endemic for leishmaniasis but
also with an epidemic of tuberculosis.
Although epidemiology and clinical examinations suggest the presence of mucocutaneous
leishmaniasis, the final diagnosis is based on the
identification of the parasite, which did not happen
in this case. The scarification smear and Giemsa
stain tests showed 75% sensitivity that decreasedas the condition evolved, reaching 20% after 6
months. Culture isolation and inoculation in hamsters showed 30% and 50% sensitivity, respectively.
The negative results of the tests in this case could
be explained by the time lapse between the onset
of symptoms and the final diagnosis (more than
2 years). Polymerase chain reaction (PCR) is a
highly sensitive molecular technique, very useful
for mucosal lesions with few amastigote forms,
but not easily available in most endemic areas. In
this particular case, the germ was not identified,
but the epidemiological and clinical diagnosis was
confirmed by serologic tests and the Montenegro
reaction. Actually, the diagnosis confirmation derived from the therapeutic response.
Leishmaniasis cases have been reported in
different parts of the world, with oral mucosa
involvement in almost every case. The World
Health Organization (WHO) estimates that 2-3%
of patients with acquired immune deficiency syndrome (AIDS) have developed leishmaniasis as
an opportunistic infection. Mucosal leishmaniasis
caused by Leishmania braziliensis is known to affect 1-10% of the cases.
Approximately 90% of patients present a prior
cutaneous scar. Occasionally, mucosal lesions may
also appear in patients with no previous skin lesions. The exclusive involvement of the mucosa
is very rare20.
In the review published in 2003 by Aliaga et al,
in 31 patients with mucosal leishmaniasis (42%
with no underlying disease, 58% with other several medical conditions), the lesions were mostly
located on the larynx (35%), oral mucosa (32%)
and the nose (16%). Tracheal lesions were not
described. Mucosal lesions were painless in allpatients, including this case. Ulcerations were reported in 6 patients. In a way similar to the biopsy
results of our patient, according to the pathologic
findings, the lesions showed chronic inflammatory
infiltrate with granulomas.
Parasites are easily identified in smears of Giemsa stain or hematoxylin and eosin stain. But
parasite growth in cultures occurs only in 60% of
the patients1.
A recent review of related literature between
1950 and 2013 of the cases of patients with primary
head-neck mucosal manifestations of leishmaniasis identified only 13 patients and showed that
the most commonly affected sites were the larynx
(54%), the mouth (31%) or the pharynx (23%) and
endonasal site (15%), with the exophytic lesion as
the most frequent clinical presentation (69%)18.
To the best of our knowledge, only four cases
of tracheal leishmaniasis have been previously
described in the literature, showing the exceptional nature of this case. Probably the delayed
diagnosis (the case was initially interpreted as
tuberculosis) justifies progression towards the
lower airway, even without involvement of the
immune system23-25.
The treatment of choice for every clinical manifestation of leishmaniasis is the administration of
antimonial drugs such as meglumine antimoniate
(Glucantime) and sodium stibogluconate (Pentostam). Meglumine is administered at a dose of 20
mg/kg of body weight/day via the intramuscular or
intravenous route, to a maximum of 850 mg/day
for at least 20 days. The possible adverse effects
of these drugs are myalgia, joint pain, anorexia,
nausea, vomiting, headache, hypertransaminasemia, chemical pancreatitis, thrombocytopenia
and neutropenia. Patients with mucocutaneous
leishmaniasis shall be treated with 20 mg of
pentavalent antimony (0.2 ml of Pentostam) per
kg of body weight daily, via the intramuscular or
intravenous route during 30 days. An intralesional
injection of sodium stibogluconate (0.5 to 1.0 ml)
could be effective. It is a less expensive alternative
with few side effects11-18.
We conclude that leishmaniasis is an endemic
parasitosis with increasing incidence. This case
stresses the importance to consider leishmaniasis
as a differential diagnosis in patients with mucosal
lesions, even without previous skin disease, since
the primary lesion in some cases may go unnoticed.
Despite its macroscopic similarities to tuberculosis,leishmaniasis shall always be suspected in patients
of endemic regions with mucosal lesions of the
trachebronchial tree.
Conflicts of Interest: the author declares there is no conflict of interest related to this publication.
1. Aliaga L, Cobo F, Mediavilla JD et al. Localized mucosal leishmaniasis due to leishmania infantum: clinical and microbiologic findings in 31 patients. Medicine (Baltimore) 2003; 82(3): 147-58.
2. Angles R, Le Pont F, Desjeux P. Visceral canine leishmaniasis in Bolivia. Trans R Soc Trop Med Hyg 1982: 76, 704.
3. Balcazar JM. Epidemiología en Bolivia. La Paz: Ediciones Juventud, 1955.
4. Balcazar JM. Historia de la medicina en Bolivia. La Paz: Ediciones Juventud, 1956
5. Costa JWJr, Milner DAJr, Maguire JH. Mucocutaneous leishmaniasis in a us citizen. Oral surgery, oral medicine, oral pathology, oral radiology, and endodontics 2003; 96(5): 573-577.
6. Delgado O, Feliciangeli MM, Gómez B, Alvarado J, García L, Bello C. The re-emergence of American visceral leishmaniasis in an old focus in Venezuela: present situation of human and canine infections. Parasite 1998; 5(4): 317-323.
7. Desjeux P, Aranda E, Aliaga O, Mollinedo S. Human Visceral Leishmaniasis In Bolivia; First proven autochthonous case from los Yungas. Trans R Soc Trop Med Hyg 1983; 77(6): 851-852.
8. Martinez E, Le Pont F, Mollinedo S, Cupolillo E. A first case of cutaneous leishmaniasis due to Leishmania (Viannia) lainsoni in Bolivia Trans R Soc Trop Med Hyg 2001; 95 (4): 375-377.
9. Desjeux P, Mollinedo S, Le Pont F, Paredes A, Ugarte G. Cutaneous Leishmaniasis In Bolivia. A Study of 185 human cases from Alto Beni (La Paz Department) isolation and isoenzyme characterization of 26 strains of leishmania brasiliensis. Trans R Soc Trop Med Hyg 1987; 81, 742-746.
10. Croft SL, Dye C, Kahl LP. Leishmaniasis: The first centenary (1885-1985) new strategies for control. Parasitology Today 1988; 4 (2): 51-53.
11. Faris RM, Jarallah JS, Khoja TA, Al-Yamani Mj. Intralesional treatment of cutaneous leishmaniasis with sodium stibogluconate antimony. International Journal of Dermatology 1993; 32(8): 610-612.
12. Forero M, Pérez A, Barajas NC, Leyva YA, Zamora C. Nasolaryngotracheal mucosal leishmaniasis in an Adolescent. Arch Argent Pediatr 2014; 112(3): E101-4.
13. Garret Aillon J. La espundia en Bolivia, observaciones del Dr. Manuel Antonio Vaca Diez. Comentario histórico. Boletín Informativo de CENETROP. IX, 1-5, 1983.
14. Gatti G, Boggino J, Prieto C. Un nouveau foyer de leishmaniose viscerale en Amerique du sud. Bulletin de la Societe de Pathologie Exotique 1939; 67, 387- 395.
15. La Fuente C, Recacochea M, Tybayrenc M, Urjel R, Darras C, Cardozo L. Leishmaniasis en Bolivia: Presencia de dos complejos en los llanos orientales del departamento de Santa Cruz-Bolivia. Boletín científico del CENETROP, vol. XII, 1-15, 1986.
16. Le Pont F, Desjeux P. 1986; Leishmaniasis In Bolivia II. The involvement of psychodopygus yucumensis and psychodopygus llanos martinsi in the selvatic transmission cycle of leishmania braziliensis in a lowland subandean region; mem. Inst. Oswaldo Cruz, Rio de Janeiro, vol. 81(3): 311-318.
17. Le Pont F.; Mollinedo S.; Mouchet J.; Desjeux P. Leishmaniose en Bolivie. IV. Le chien dans les cycles des leishmanioses en Bolivie. Rio de Janeiro: Inst. Oswaldo Cruz 1989, vol. 84 (3) pp 417-421.
18. Leishmania species of all major complexes may be responsible for ml over the world. World health organization, “world health organization working to overcome the global impact of neglected tropical disease,” first who report on neglected disease, World Health Organization, Geneva, Switzerland, 2010.
19. Marshall BG, Kropf P, Murray K et al. Bronchopulmonary and mediastinal leishmaniasis: an unusual clinical presentation of Leishmania donovani infection. Clin Infect Dis 2000; 30(5): 764-9.
20. Mignogna MD, Celentano A, Leuci S et al. Mucosal leishmaniasis with primary oral involvement: a case series and a review of the literature. Oral Dis 2015; 21(1): e70-8.
21. Mollinedo S, Muñoz M, Hervas D et al. Leishmaniasis visceral y tegumentaria en niños en dos zonas endémicas de Bolivia. Parasitología al día 1992; 16: 11-120.
22. Murray HW, Berman JD, Davies CR, Saravia NG. Advances in Leishmaniasis. The Lancet 2005; 366(9496): 1561-1577.
23. Piens MA, Arpin D, Rabodonirina M, Loire R, Brune J. Tracheal stenosis of inflammatory aspect. Rev Pneumol Clin 1997; 53(3): 150-2.
24. Valda l. Leishmaniasis cutáneo difusa: informe del segundo caso boliviano; Cuadernos del Hospital de Clínicas 1980; 31,1.
25. Viglianesi A, Di Mauro D, Petrillo G. Multidetector computed tomography aspects of tracheal mucosal leishmaniasis localization Jpn J Radiol 2011;29(1): 59-62.