Autor :Herrero MarÃa Victoria1, Faggionato Martina1, Cigarra Cecilia Mariela1, Rigoni MarÃa Luz1, de la Cruz Mariano AgustÃn1, DÃaz Ballvé Pablo2
1Hospital Petrona Villegas de Cordero, San Fernando, Pcia Buenos Aires, Argentina 2 Hospital Profesor Alejandro Posadas, El Palomar, Pcia Buenos Aires, Argentina
Correspondencia : Herrero, MarÃa Victoria; e-mail: residenciakinesiosanfer@yahoo.com.ar
Abstract
Objectives: To compare and establish the degree of agreement between the values of Maximal Inspiratory Pressure (MIP) and Maximal Expiratory Pressure (MEP) measured with a plastic mouthpiece and a scuba type mouthpiece in adults. The secondary objective was to evaluate the degree of agreement between the values calculated with the equations by Evans and Whitelaw and the maximal values attained with each interface.
Materials and Method: We conducted an observational, descriptive, prospective transversal study. We carried out a consecutive, non-probabilistic sampling of Argentinian subjects aged between 18 and 69 years. We measured the MIP and MEP with a unidirectional valve system and an aneroid manovacuometer, with a plastic mouthpiece and a scuba type mouthpiece.
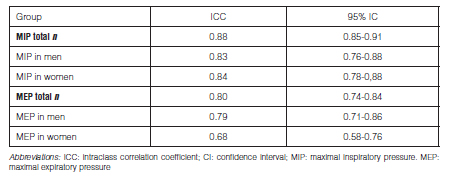
Results: A total of 240 subjects were included and completed all the measurements with both interfaces. MEP values were higher when measured with a plastic mouthpiece compared to the scuba type (p < 0.01), with an Intraclass Correlation Coefficient (ICC) between them of 0.80 (95% CI [confidence interval]: 0.74-0.84). There were no differences in the MIP between both interfaces, with an ICC of 0.88 (95% CI: 0.85-0.91). The ICC between the equations by Evans and Whitelaw and the maximal values attained by the subjects varied from -0.15 to 0.09, showing a low degree of agreement.
Conclusion: MEP values attained with a plastic mouthpiece are greater than those attained with the scuba type mouthpiece. There are no differences between both interfaces for the MIP. Evans and Whitelaw equations were not successful in predicting maximal pressures in the population under study.
Key words: Mouthpiece; Respiratory muscles; Maximal respiratory pressures.
Introduction
The measurement of pressures generated at the mouth level during maximal respiratory efforts is a simple way to evaluate the strength of inspiratory and expiratory muscles. This measurement can be performed through noninvasive, well-tolerated examinations by which it is possible to know the maximal static inspiratory pressure (MIP) and the maximal static expiratory pressure (MEP) that a person can generate during an effort1, 2. In these tests, the patient generates the maximal inspiratory and expiratory pressures against a closed system that translates such effort into an absolute value. Measuring these pressures is very useful from the clinical point of view for the diagnosis and follow-up of diseases affecting the respiratory muscles1, 3.
The device necessary to perform the measurements is an interface connected to a small camera with a valve system linked to a pressure transducer, that can be aneroid or digital4. The system needs an exit site with an internal diameter of approximately 2 mm in order to prevent the glottic closure during the MIP measurement and reduce the use of the mouth’s muscles during the MEP maneuver1, 2. There is a broad variety of interfaces that can be used for this maneuver. The literature has described the use of the scuba type mouthpiece1-2, 5-9, the cylindrical mouthpiece5, 7, 10-14, and the plastic mouthpiece9, and there is even some evidence of authors who have performed such measurements with a mask10, 15-16.
By convention, and in order to standardize the measurements, the MIP is measured starting from the residual volume or the closest value, and the MEP is measured starting from the total lung capacity or the closest value1, 14. As regards the amount of measurements needed in an evaluation, the American Thoracic Society (ATS) and the European Respiratory Society (ERS) suggest performing 3 maneuvers as a maximum, with less than 20% variability between them. Also, they have established previous training guidelines and instructions1. Various studies have reported normality ranges and regression equations that allow for the estimation of MIP and MEP values in healthy subjects1-2, 5-6, 11, 14, 17-19. The equations we use in our institution are those formulated by Evans and Whitelaw in 2009. These authors, just like the ATS and the ERS, recommend the use of the scuba type mouthpiece. Those equations are divided by gender and take into account the age of the subjects, showing little variation until 69 years. They also include formulae to calculate the Lower Limit of Normal (LLN) of each maneuver1-2.
With respect to the previously described mouthpieces, in our workplace we use the hard plastic mouthpiece, which we can easily get since it can be found within the nebulizer set. Also, this interface has the advantage of being economical and sterilizable. Though we do not have an analysis of registered objective data, we have observed in the daily practice that when performing MIP and MEP measurements with the plastic mouthpiece, the frequency of perioral air leaks seemed to be lower compared to the scuba type mouthpiece. On the other hand, the values reached by our patients in several occasions exceeded the calculated theoretical values, regardless of the interface. Since we haven´t found any evidence of the use of a plastic mouthpiece with an aneroid manovacuometer, we developed a study whose primary objective is to compare and establish the degree of agreement between the MIP and MEP values measured with a plastic mouthpiece and a scuba type mouthpiece in adults. The secondary objective is to evaluate the degree of agreement between the theoretical values calculated with the formula by Evans and Whitelaw and the maximal values attained with each interface.
Materials and Method
We conducted an observational, descriptive, prospective transversal study. This study has been authorized by the Teaching and Research Committee, the Bioethics Committee and the Hospital Management.
Setting: measurements were taken between December, 2015 and December 2016 in the gymnasium and outpatient service area of the Kinesiology Inpatient Care Unit.
Subjects: the study participants were registered through consecutive, non-probabilistic sampling. Inclusion criteria: Caucasian subjects aged between 18 and 69 years who verbally declared they were not suffering acute or chronic respiratory diseases the moment the measurements were taken. Exclusion criteria: subjects who claimed to have alterations in the chest wall, cardiovascular diseases, neurologic disorders or neuromuscular diseases; or those going through an immediate post-surgical period, or with difficulty to achieve complete lip closure; and subjects who did not agree to sign the informed consent. In order to maintain the anonymity of participants and guarantee the reliability of the data, we assigned a number to each subject.
Variables: the primary variables of the study were the MIP and the MEP, defined as the maximal inspiratory and expiratory static pressures registered during a maximal voluntary effort. To take the measurements we used a Meco® manovacuometer with a pressure range ± 150 cmH2O and recordings every 2.5 cmH2O, using a continuous quantitative scale. The device had been previously calibrated by the manufacturer at the beginning of the study by the water column method in ascending and descending values of pressure and vacuum; then, we followed the frequency recommended by him for recalibration. The secondary variables were: age, in years (discrete quantitative scale), gender (dichotomous qualitative scale), weight in kilograms (discrete quantitative scale), height in meters (continuous quantitative scale) and mass body index defined as the result of weight in kilograms divided by the square of height in meters (continuous quantitative scale).
To take the measurements, we used a unidirectional valve system based on the model described by Arce and De Vito20 (Figure 1). The mouthpieces that we used were the IST® silicone scuba type mouthpiece, model MP-1 (Figure 2) and the plastic mouthpiece included in the Hudson RCI® nebulizer set, model Micro Mist (ref. 1882) (Figure 3). They both present an adjustable 22 mm connector.
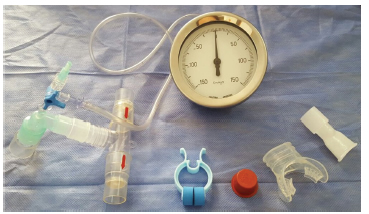
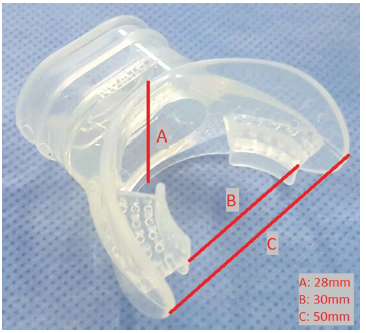

Randomization: measurements were divided in 4 groups according to requested effort and interface to be used. MIP with plastic mouthpiece (MIPPM), MIP with scuba type mouthpiece (MIPSM), MEP with plastic mouthpiece (MEPPM) and MEP with scuba type mouthpiece (MEPSM). These 4 groups can be combined in 24 different ways so that measurements can be carried out in every possible order. That is why the order of the maneuvers was randomized in blocks of 24 different combinations, placing each assigned order in a closed opaque envelope. Each subject took an envelope after being included in the study.
Sample size and power: The sample size was defined in 240 subjects, after repeating 10 times the randomized blocks of 24 possible combinations. With this n, 98% power was achieved, assuming an alpha error of 5% for a minimum expected difference of 10 cmH2O for both methods (SD ± 27 cmH2O). Dispersion was obtained out of a pilot sample of 48 subjects (2 blocks of 24).
Procedure: all of the subjects remained seated on a chair with their hands on their thighs and their arms in a relaxed position, holding their back against the back of the chair and their feet on the floor. A nose clip was placed to avoid leaks and the subjects were only allowed to use their hands to adjust the plastic or scuba type mouthpiece inside their mouth. Once the mouthpiece was adjusted, the subjects were asked to provide the MIP and MEP effort according to the randomized maneuvers. Before taking the measurements, the following instructions were explained to the subjects: “During repetitions, you must close your lips strongly to avoid air leaks around the plastic or scuba type mouthpiece, and if you actually feel there is a leak, you must inform us. Since our objective is to record the highest pressures you are able to achieve, we will encourage you during every repetition and will tell you when to stop the effort. You will be given a break between each repetition and you must inform us if there is any kind of discomfort or problem to continue”.
Before each maneuver, the following instructions were given: MIP: “Make a maximal expiration followed by the greatest inspiratory effort you can make. At this time, the system will let you breathe out but not in.” MEP: “Breathe in as much air as you can and then put forth your maximum expiratory effort. At this time, the system will let you breathe in but not out”. We defined words of motivation that were repeated continuously during the MIP and MEP maneuvers: “Breathe in deep, deep, deep!” and “Blow strong, strong, strong!”, respectively.
Every subject performed the necessary repetitions until 3 measurements were recorded, with less than 20% variability between them. Data was recorded in two forms: Form A, of individual use, for personal data, the assigned order and the values achieved in every MIP and MEP repetition with both interfaces; and Form B, of general use, containing all the data from Form A and the theoretical pressure values according to the Evans and Whitelaw equations for each subject.
The evaluators were physiotherapists trained in taking measurements. There were two professionals per each measurement. One was in charge of holding the valve system in front of the subject, controlling the correct development of the technique and verbal motivation; whereas the other physiotherapist recorded in the individual form the maximum value reached in the manovacuometer for each repetition, ensuring that the variation was lower than 20%. Every effort was considered as finished if, after at least 5 seconds, the peak pressure had not been exceeded. We established a one minute break between each repetition, and a three minute break between each effort group.
The assessed subjects who did not reach the LLN suggested by the Evans and Whitelaw formulae, were referred to the Neumotisiology Service in order to discard associated respiratory disease by means of a spirometry.
Statistical Analysis: continuous numerical variables were expressed through measures of central tendency and dispersion according to the presented distribution. The variables measured in categorical scale are represented as absolute frequency and its percentage by category. In order to define the normality of continuous variables we used the Kolmogorov-Smirnov test. To compare continuous variables, we used the Wilcoxon test for dependent samples, and to compare categorical variables, the Chi2 test or the Fisher’s exact test, according to the structure of the crosstable. The comparison between the order in which measurements were taken and the values obtained was analyzed by means of a one-factor ANOVA test. The intraclass correlation coefficient (ICC) was calculated to establish the degree of agreement between both methods21,22, and we used the Bland-Altman23 graphic to analyze the behavior of the measurements taken with plastic or scuba type mouthpieces (inspiratory and expiratory) to detect systematic mistakes. We also estimated the ICC to establish the degree of agreement between the theoretical values calculated with the Evans and Whitelaw formula and the maximal values attained with each interface in men and women. For statistical purposes, a value of p < 0.05 was defined as significant. The statistical analysis was made with the IBM SPSS Statistics Base software, version 22.0 for Windows.
Results
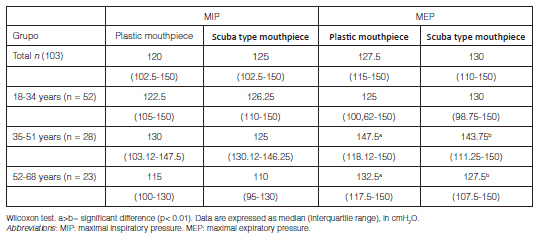
A total of 240 subjects were included and completed all the measurements. No subject was excluded or removed. Demographic and anthropometric data can be observed in Table 1.
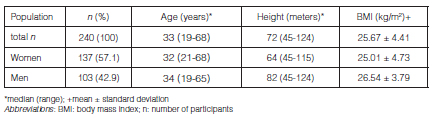
By means of the Wilcoxon test, we found statistically significant differences between MEPSM and MEPPM, with highest values obtained with the plastic mouthpiece (p < 0.001). However, there were no differences when comparing the MIP values with such interface (p = 0.44). We made a subgroup analysis per gender and age, with the purpose of investigating the behavior of these differences (Tables 2 and 3).
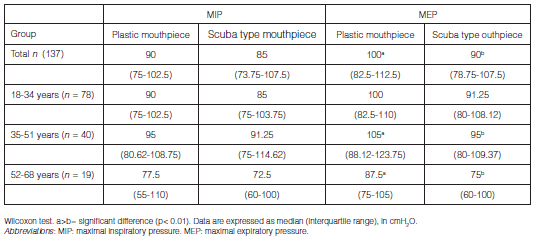
Regarding the possible influence of the assigned order of the maneuvers on the obtained values, we observed that the global MEPSM values were higher when carried out in the first order, in comparison with the third and fourth order (p < 0.01). When analyzing this data in the subgroups under study, we noted that the findings maintained their statistical significance only in women. In the case of the MIP, we observed higher values with the MIPPM as the last maneuver only in men.
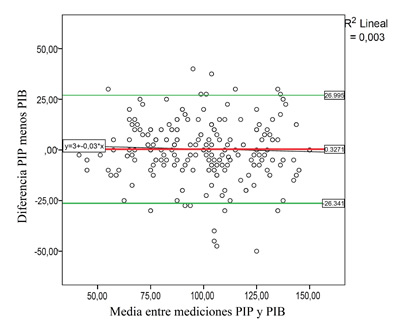
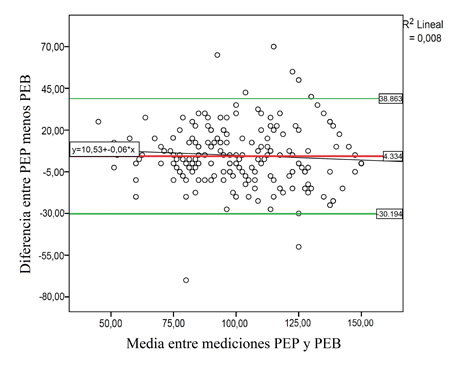
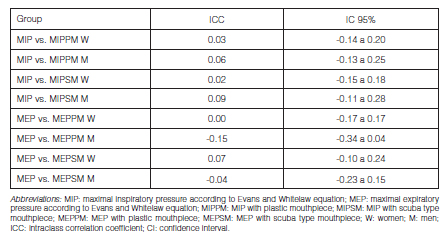
When evaluating the degree of concordance between the two interfaces, we obtained ICCs of almost perfect agreement for MIP and substantial agreement for MEP, according to the Landis and Koch24 classification (Table 4). On the other hand, Figures 4 and 5 show the Bland-Altman analysis for the MIP and MEP maneuvers, respectively.
In the analysis of concordance between the obtained values and the values calculated by the Evans and Whitelaw equations, we achieved an ICC with a “Poor” degree of agreement (Table 5).
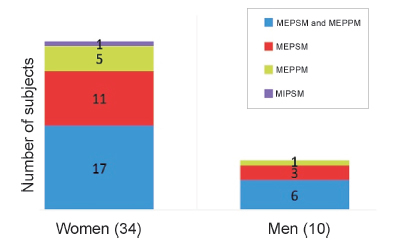
Among the pressures obtained, 44 subjects (18.33% of the total population) did not get to the LLN suggested by the Evans and Whitelaw formula (Figure 6). We performed spirometries in 31 of these individuals, obtaining normal values in every case.
Discussion
The results of our study show that MEP values using a plastic mouthpiece are higher than those with a scuba type mouthpiece. However, the MIP values did not show any differences between both interfaces, thus the type of interface to be used was chosen by the evaluator, taking into account the comfort of the patient.
These results agree with previous research, which compared the use of a scuba type mouthpiece with different types of rigid, tubular interfaces5, 7, 8. Koulouris et al conclude that the use of the scuba type mouthpiece underestimates not only the MEP but also the MIP values in healthy subjects8. However, Montemezzo et al compared in 2012 the use of the same plastic mouthpiece of our study with a scuba type mouthpiece and did not obtain any differences when taking the measurements with a digital manovacuometer9.
The ATS/ERS guidelines recommend the use of the scuba type mouthpiece, since it ensures there will be less leaks and improves comfort, mostly in subjects with oral muscle weakness1. But other authors report that lower values with the same interface may be due to the existence of perioral leaks5, 25. On the other hand, Rubinstein et al state that differences may be paralleled if the oral cavity is manually sealed with the scuba type mouthpiece7.
Windisch and Evans mention in their articles that the peak pressure can be much easily calculated than the trough pressure, since it does not need computer software and can be measured by means of an aneroid manovacuometer2, 17. Whereas some authors like Arce and De Vito suggest measuring the trough pressure value in a second with an aneroid manovacuometer20, in our study we did not find the way to do so without producing a greater measurement bias. In turn, it has been reported that the trough pressure in healthy subjects corresponds to 82-86.3% of the peak pressure in the MIP17.
We have observed that women obtained lower static pressure values: MIP, 68-75% and MEP, 69-78% of the values registered in men. These ranges are similar to those reported by various authors2, 6, 11, 14, 18, 26, 27.
Some studies have reported the existence of a learning effect with the MIP maneuver28-30. However, the only case in which we found this tendency was the subgroup of men using the plastic mouthpiece.
Normal parameters and regression equations for MIP and MEP are different according to various authors2, 6, 11, 14, 17-18, 26, 28, 31-33, and at present there is standardized consensus regarding the reference values to be used2. The only equations we found with their respective LLNs for MIP and MEP were those published by Enright and Evans and Whitelaw2, 31. In this study, we assessed concordance with the formulae described by Evans and Whitelaw since to the best of our knowledge those are the only ones that allow for the calculation of the expected MIP and MEP values and their respective LLNs in healthy men and women up to 69 years old2, 34. On the other hand, Enright equations have been formulated for subjects older than 65 years old31; and other authors have published LLN values but only for the MIP11, 17-18, 32.
It is important to focus on the fact that for the development of the equations, Evans and Whitelaw have taken into account information of other authors who had used both aneroid and digital manovacuometers. At the same time, in order to generate the LLN, they have included the values obtained with 1.96 SD below the mean value, even when the same authors have suggested the use of the 5th percentile2. We believe this could result in the LLN values underestimating the real values in some cases.
The LLNs formulated by Evans and Whitelaw are based on statistical definitions of other studies in healthy subjects, where 5% of those subjects did not reach such theoretical limits. This is why it is essential that the values obtained are interpreted in relation to the clinical situation of each individual, since there could be subjects without any kind of disease with records that do not reach the LLN2. In contrast to the 5% suggested by Evans, in our study, 18.33% of subjects (n= 44) did not reach the corresponding LLNs in at least one of four maneuvers. We haven’t observed any respiratory functional causes that justify these findings, since all the subjects claimed to be healthy and all the spirometries performed were within normal limits. It is worth mentioning that, except for one individual, the rest of the cases occurred during the MEP measurement, where the oral leakage during the maneuver or the fact that LLN values for MEP were too high for our population could be attributed to a mistake in the technique.
There is evidence that the values of respiratory pressures differ according to the different ethnic groups, countries or even regions within the same country35-36. In accordance with our results, the Evans and Whitelaw equations did not show concordance with the values obtained in our samples, thus they could not be compared. Also, we haven’t found any studies suggesting regression formulae or regional normal values, so the line of research continues towards the formulation of equations for both interfaces used with an aneroid manovacuometer.
Limitations: one of the limitations of this study was the abnormal distribution in the age variable; this may be due to the recruitment method and we believe it could be solved with randomized sampling. In addition, we have taken into account the information provided by the subject regarding the existence or non-existence of a pathological history, with the possibility of there being ill subjects unaware of their condition. There was another limitation regarding the instruments, as the manovacuometer that was used does not allow for the recording of values higher than ±150 cmH2O, and this could have influenced the results. In spite of this limitation, we think the values of greatest relevance in the clinical practice are those below the lower limit of each subject. As regards the reproducibility of measurements, various authors have reported almost perfect reliability values with digital and aneroid manovacuometers30, 35, 37-40. We haven’t found a consensus regarding the specific instructions and motivation words intended for the subjects, so we designed a protocol based on recommendations and our own experience. Just like Evans, we believe the details regarding how the test is carried out, from the election of the interface to the instructions, motivation and analysis of the data, generate important differences in the result, thus their standardization is essential2.
Conclusion
We may conclude that MEP values attained with a plastic mouthpiece are higher than those attained with the scuba type mouthpiece. In the case of the MIP, there are no differences between both interfaces. The pressure values attained and the ones estimated by the Evans and Whitelaw formulae had a poor correlation. Considering these equations were not successful when predicting the MIP and the MEP, it would be useful to formulate regression equations for the population under study.
We believe we need future research to have more information about the use of the plastic mouthpiece and the scuba type mouthpiece for the measurement of the MIP and MEP and their regional lower limits of normal.
1. Green M, Road J, Sieck GC, Similowski T. American Thoracic Society/European Respiratory Society. Statement on Respiratory Muscle Testing. Am J Respir Crit Care Med. 2002; 166: 518-624.
2. Evans JA, Whitelaw WA. The assessment of maximal respiratory mouth pressures in adults. Respir Care. 2009; 54 (10): 1348-1359.
3. Mora-Romero UJ, Gochicoa-Rangel L, Guerrero-Zúñiga S, et al. Presiones inspiratoria y espiratoria máximas: recomendaciones y procedimiento. Neumol Cir Torax. 2014; 73 (4) : 247-253.
4. De Souza RB. Diretrizes para Testes de Função Pulmonar. J Pneumol. 2002; 28 Suppl 3: S155-165.
5. Szeinberg A, Marcotte JE, Roizin H et al. Normal values of maximal inspiratory and expiratory pressures with a portable apparatus in children, adolescents, and young adults. Pediatric pulmonology. 1987; 3: 255-258.
6. Wilson SH, Cooke NT, Edwards RHT, Spiro SG. Predicted normal values for maximal respiratory pressures in caucasian adults and children. Thorax. 1984; 39: 535-538.
7. Rubinstein I, Slutsky AS, Rebuck AS, et al. Assessment of maximal expiratory pressure in healthy adults. J Appl Physiol. 1988; 64 (5): 2215-2219.
8. Koulouris N, Mulvey DA, Laroche CM, Green M, Moxham J. Comparison of two different mouthpieces for the measurement of PImáx and PEmáx in normal and weak subjects. Eur Respir J. 1988; 1: 863-867.
9. Montemezzo D, Rocha Vieira D, Tierra-Criollo C, Rodrigues Britto R, Velloso M, Franco Parreira V. Influence of 4 interfaces in the assessment of maximal respiratory pressures. Respir Care. 2012; 57 (3): 392-398.
10. Wohlgemuth M, van der Kooi EL, Hendrinks JC, Padberg GW, Folgering HT. Face mask spirometry and respiratory pressures in normal subjects. Eur respire J. 2003; 22: 1001-1006.
11. Hautmann H, Hefele S, Schotten K, Huber RM. Maximal inspiratory mouth pressures (PIMÁX) in healthy subjects – what is the lower limit of normal? Respiratory Medicine. 2000; 94: 689-693.
12. Fiz JA, Carreres A, Rosell A, Montserrat JM, Ruiz J, Morera JM. Measurement of maximal expiratory pressure: effect of the holding lips. Thorax. 1992; 47: 961-963.
13. Tully K, Koke K, Garshick E, Lieberman SL, Tun CG, Brown R. Maximal expiratory pressures in spinal cord injury using two mouthpieces. Chest. 1997; 112: 113-116.
14. Black LF, Hyatt RE. Maximal respiratory pressures: normal values and relationship to age and sex. Am Rev Respir Dis. 1969; 99: 696-702.
15. Ratnovsky A, Elad D, Zaretsky U, Shiner RJ. A technique for global assessment of respiratory muscle performance at different lung volumes. Physiol. Meas. 1999; 20: 37-51.
16. Fregadolli P, Sasseron AB, Cardoso AL, Veloso Guedes CA. Respiratory pressures evaluation on healthy subjects by mouthpiece and facemask. Rev Bras Clin Med. 2009; 7: 233-237.
17. Windisch W, Hennings E, Sorichter S, Hamm H, Criée CP. Peak or plateau maximal inspiratory mouth pressure: which is best? Eur Respir J. 2004; 23: 708-713.
18. Harik-Khan RI, Wise RA, Fozard JL. Determinants of maximal inspiratory pressure. The Baltimore Longitudinal Study of Aging. Am J Respir Crit Care Med. 1998; 158: 1459-1464.
19. Sclauser Pessoa IMB, Franco Parreira V, Fregonezi GAF, Sheel AW, Chung F, Reid WD. Reference values for maximal inspiratory pressure: a systematic review. Can Respir J. 2014; 21 (1): 43-50.
20. Arce SC, De Vito EL. Construcción de válvula unidireccional para la determinación de presiones bucales máximas. [Internet series]. [cited February 22, 2017]; [approx. 4 p.]. Available at: http://www.aamr.org.ar/secciones/fisiopatologia_lab_pulmonar/construccion_valvula_unidireccional.pdf
21. Fleiss JL, Cohen J. The equivalence of weighted kappa and the intraclass correlation coefficient as measures of reliability. Educ Psychol Meas. 1973; 33: 613-9.
22. Kramer MS, Feinstein AR. Clinical biostatistics LIV. The bioestatistics of concordance. Clin Pharmacol Ther. 1981; 29: 111-123.
23. Bland A, Altman D. Comparing methods of measurement: why plotting difference against standard method is misleading. Lancet. 1995; 346: 1085-1087.
24. Landis JR, Koch GG. The measurement of observer agreement for categorical data. Biometrics. 1977; 33 (1): 159-174.
25. Cook C, Mead J, Orzalesi MM. Static volume pressure characteristics of the respiratory system during maximum efforts. J Appl Physiol. 1964; 19: 1016-1021.
26. Neder JA, Andreoni S, Lerario MC, Nery LE. Reference values for lung function tests. II. Maximal respiratory pressures and voluntary ventilation. Braz J Med Biol Res. 1999; 32: 719-727.
27. Lausted C, Johnson A, Scott W, Johnson M, Coyne K, Coursey D. Maximum static inspiratory and expiratory pressures with different lung volumes. BioMedical Engineering OnLine [Internet series]. May 2006. [cited February 22, 2017]; [approx. 6 p.]. Available at: http://biomedical-engineering-online.biomedcentral.com/articles/10.1186/1475-925X-5-29.
28. Bruschi C, Cerveri I, Zoia MC et al. Reference values of maximal respiratory mouth pressures: A population-based study. Am Rev Respir Dis. 1992; 146: 790-793.
29. Wen AS, Woo MS, Keens TG. How many maneuvers are required to measure maximal inspiratory pressure accurately? Chest. 1997; 111: 802-807.
30. Dimitriadis Z, Kapreli E, Konstantinidou J, Oldham J, Strimpakos N. Test/retest reliability of maximum mouth pressure measurements with the MicroRPM in healthy volunteers. Respir Care. 2011; 56 (6): 776-782.
31. Enright PL, Kronmal RA, Manolio TA, Schenker MB, Hyatt RE. Respiratory muscle strength in the elderly. Correlates and reference values. Cardiovascular Health Study Research Group. Am J Respir Crit Care Med. 1994; 149: 430-438.
32. Sachs MC, Enright PL, Stukovsky KH, Jiang R, Barr RG. The Multi-ethnic Study of Atherosclerosis (MESA) Lung Study. Performance of maximal inspiratory pressure tests and MIP. Reference equations for four ethnic groups. Respir Care. 2009; 54(10): 1321-1328.
33. Costa D, Goncalves HA, Lima LP, Ike D, Cancelliero KM, Montebelo MI. New reference values for maximal respiratory pressures in the Brazilian population. J Bras Pneumol. 2010; 36: 306-312.
34. Petrini M, Haynes D. In search of maximum inspiratory and expiratory pressure reference equations. Respiratory Care. 2009; 54(1): 1304-1305.
35. Franco Parreira V, França DC, Zampa CC, Fonseca MM, Tomich GM, Britto RR. Maximal respiratory pressures: actual and predicted values in healthy subjects. Rev. Bras. Fisioter. 2007; 11 (5): 361-368.
36. Barreto LM, Duarte MA, Costa Drumond de Oliveira Moura S, Alexandre BL, Silva Augusto L, Fernandes Fontes MJ. Comparison of measured and predicted values for maximum respiratory pressures in healthy students. Fisioter Pesq. 2013; 20 (3): 235-243.
37. Larson JL, Covey MK, Vitalo CA, Alex CG, Patel M, Kim M. Maximal inspiratory pressure: learning effect and test retest reliability in patients with chronic obstructive pulmonary disease. Chest. 1993; 104: 448-453.
38. Jalan NS, Daftari SS, Retharekar SS, Rairikar SA, Shyam AM, Sancheti PK. Intra- and inter-rater reliability of maximum inspiratory pressure measured using a portable capsule-sensing pressure gauge device in healthy adults. Can J Respir Ther. 2015; 51(2): 39-42.
39. Sclauser Pessoa IMB, Alves Pereira HL, Tavares Aguiar L, Leite Tagliaferri T, Mendes da Silva LA, Franco Parreira V. Test-retest reliability and concurrent validity of a digital manovacuometer. Fisioter Pesq. 2014; 21 (3): 236-242.
40. Wilches-Luna EC, Sandoval LM, López DJ. Confiabilidad intra e inter evaluador de la medición de la presión inspiratoria máxima (Pimáx) en treinta sujetos sanos de la ciudad de Cali. Rev Cienc Salud. 2016; 14 (3): 329-338.