Autor : Borsini Eduardo1, 2, Ernst Glenda1, 2, Blanco MagalĂ1, 2, Di Tullio Fernando1, DecimaTamara1, Robaina Gabriela1, Campos JerĂłnimo1, Bosio MartĂn1, Meraldi Ana1, Blasco Miguel1, Salvado Alejandro1
1 Center for Respiratory Medicine. Hospital Británico de Buenos Aires 2Sleep and Ventilation Unit. Hospital Británico de Buenos Aires
Correspondencia : Eduardo Borsini borsinieduardo@yahoo.com.ar
Abstract
Introduction: Continuous positive airway pressure (CPAP) has proven to be effective
in the treatment of obstructive sleep apnea/hypopnea syndrome (OSAHS). Effective
pressure is traditionally acquired with a polysomnography (PSG). The performance of
unconventional strategies, such as auto-adjusting positive airway pressure (APAP) and
titration formulas (Tf) varies according to the population where they are applied.
Objective: To describe the APAP titration and correlate the mean airway pressure (Meanp),
the Effp and the Hoffstein and Mateika Tf pressure
(Hofff).
Results: We included 192 patients, 52 female (27%) and 140 male; age, 60.2 years
old ± 11.7 and BMI (body mass index) of 33.8 ± 6.7 kg/m2. The apnea-hypopnea index
(AHI) was: 33.1 ± 16.6 in females and 36.5 ± 16 in males (p > 0.24); and 190 cases
(98.9%) had an AHI > 15 ev/hour. Mean compliance with APAP was: 380 minutes ± 101
in females and 370 ± 91.2 in males (p > 0.54). Less than 10% of the population presented
unacceptability criteria.
We found a correlation between the Meanp and the Effp; rho: 0.73 (95% CI [confidence
interval] 0.57-0.84) p < 0.001. However, between the Effp and the Hofff β: 0.519 and
r2: 0.269 (p < 0.001) there was an underestimation by Hofff: - 1.98 cm H2O (95% CI,
1.48-2.49) and intraclass correlation index: 0.60 (95% CI: 0.47-0.80) p < 0.0001.
Conclusions: A high proportion of patients titrate at home with APAP without supervision and with acceptability criteria. We did not find a suitable correlation between the
Hofff and the Effp in our population.
Key words: Titration; CPAP; Hoffstein and Mateika
Introduction
The obstructive sleep apnea/hypopnea syndrome
(OSAHS) is a clinical condition characterized
by recurrent episodes of upper airway obstruction during sleep. The evidence gathered up to
now demonstrates that the OSAHS without a
suitable treatment is associated with arterial
hypertension, stroke, deterioration in quality
of life, traffic accidents and a higher risk of dying due to cardiovascular events1-5. Continuous
positive airway pressure (CPAP) has proven to be the most effective treatment modality, since
it corrects obstructive events during sleep and
intermittent hypoxemia, and improves the sleep
structure and quality of life of the affected individuals6-8.
Once the OSAHS diagnosis has been established
by means of polysomnography (PSG) or respiratory
polygraphy (RP), if the patient complies with the
criteria to use the CPAP, some method shall be
used to define the pressure values to be set in the
equipment that will be used by the patient at home
(titration procedure).
The effective pressure is traditionally acquired
with a second nocturnal PSG7-11 or during the same
night in which the diagnosis is established with
the known split-night PSG12-14.
The proposal to use auto-adjusting or automatic
CPAP equipment (APAP) as an unconventional titration method comes from centers with a great demand
of sleep studies and long waiting lists. Though the
auto-adjusting equipment was not originally designed to this end, the method has spread thanks to
its capacity to register in its memory working pressure variations throughout the night in response to
airway obstruction phenomena, making it possible
to analyze the behavior of that variable according to
the requirements of the patient during sleep.
APAP titration can be used at the patient´s
home for several nights, thus increasing the range
of registered data, making it possible to observe
variations night after night, and reducing the waiting list and operational costs of the conventional
titration procedure15-19.
The last update of the American Academy of Sleep
Medicine (AASM) recommendations considers the
APAP titration as a valid option for patients with no
significant comorbidities, but it recommends manual
data analysis by experienced personnel20. The practical guidelines of the Argentinian Association of
Respiratory Medicine (AAMR, by its acronym in
Spanish) acknowledge the usefulness of this procedure to titrate the pressure level at the sleep lab or“during one or several nights at the patient´s home
with no supervision or additional monitoring”21.
There are remarkable differences among the
different algorithms validated and proposed by the
manufacturers of different equipment brands, so it
is necessary to use the algorithms that have been
compared with conventional titration PSG20-21.
On the other hand, experience with predictive
titration formulas (Tf) based on anthropometric
or clinical parameters varies according to the
population where it is applied22. Since there are
no validations of a Tf in our country, we recommended the correlation of pressures suggested
by the algorithm of an APAP model in relation to
predictive formulas and to the final recommendation of effective pressure (Effp).
Objective
To describe our experience with APAP titration in patients with OSAHS who have no experience in the use of CPAP, and to establish the relationship between the airway mean pressure (Meanp) calculated by the APAP, the Effp defined by experts, and pressures calculated by the Hoffstein and Mateika titration formula22 (Hofff).
Study Design
Prospective, correlational study at a single center.
Materials and Methods
Population
Prospective study based on home APAP titrations
of systematic collection made between August,
2015 and August, 2016 (one year) in patients with
OSAHS referred to the Sleep Unit for interface
demonstration and unsupervised home titration.
We only considered the records of patients with no
previous experience in the use of the device. The
authors did not participate in the indication of the
CPAP, which was made by the respective attending
pulmonologists.
Patients diagnosed with obesity hypoventilation
syndrome, periodic breathing or central apneas on
the baseline study and those who required other
treatment modalities (ventilation with two pressure levels, servo-controlled ventilation, concomitant oxygen use) were not included in the study.
The baseline apnea-hypopnea index (AHI) was
obtained from the PSG or RP records and anthropometric parameters; the body mass index (BMI)
and neck circumference (Ncirc) were calculated
before delivery of the CPAP device.
Auto-adjusting CPAP titration
The mask type, size and model were selected after
an interface demonstration carried out by physiotherapists with experience in sleep medicine.
The final selection of the mask depended on the
patient´s preferences and the leakage test with
the APAP equipment after a ≈ 30 minutes test.
Every patient received basic instructions regarding
the operation of the CPAP device together with
their partner or roommate. The patients were also
invited to participate in the educational program
called “CPAP school”.
System One (Philips-Respironics) auto-adjusting devices were used. Unlike the conventional
CPAP, which operates with a positive pressure
fixed value, this algorithm automatically modifies pressures with a built-in flow sensor and adjusts
working pressure according to the presence of
apneas, limitation to inspiratory flow and snoring
until a normal breathing pattern is allowed23. The
minimum pressure was set to 4 cm of H2O and
the maximum pressure to 15 cm of H2O. No ramp
features, expiratory pressure relief or thermohumidifiers were used.
The titration period coincided with the current
processes of the Sleep Unit (3 to 7 days), depending
on the appointment and device availability.
Titration data were obtained after downloading the information from the CPAP memory (SD
card) with the Encore pro II Philips-Respironics
software.
The effective pressure data were obtained after the subjective visual analysis of the pressure/time curve night after night made by physicians
and physiotherapists with experience in sleep
medicine, excluding leakage periods of more
than 25 liters/minute (compensation limit of the
equipment). The resulting final effective pressure
was selected taking into account the nights with
greater use and less leakages.
> 6500 hours of APAP use recording were
analysed. Compliance, mean leakage and residual
apnea-hypopnea index (rAHI) data were gathered.
Minimum compliance (Minc) was defined as the
use of at least 4 hours per night, taking into account the total number of nights with effective
use of CPAP, and optimum titration (OPTt) was
defined as that with rAHI < 5 events per hour (ev/hour) and minimum compliance. When the rAHI
was between 5 and 10 ev/hour, the titration was
considered as acceptable. Finally, the titration was
considered inadequate (Inadt) when there was a
rAHI of more than 10 ev/hour, with a compliance of< 4/hours per night, or when there were leakages
above the compensation limit > 50% of the nights.
The data of the EFFp reading made by experts in
relation to the automatic data of the APAP (Meanp of the first day, Meanp of every day) were compared
with the pressure previously stated by the Hofff(22),
namely: (0.16 x BMI + 0.13 x Ncirc in centimeters
+ 0.04 x baseline AHI – 5.12 = effective pressure).
Statistical Analysis
Results were presented as percentages for the
categorical variables or as mean and standard
deviation (±) for the numerical variables. For
the comparison of differences, we used the Mann-Whitney or Fisher tests or χ2. For the comparison
of titration pressures we carried out Bland and Altman plot representation, linear regression analysis
and calculation of the intraclass correlation coefficient (ICC). For the statistical analysis, STATA
12 and Graph Pad Prism-5™ software were used.
Results
During 12 moths, we included 192 patients; 52 females (27%) and 140 males; mean age, 60.2 years old ± 11.7 and mean BMI of 33.8 ± 6.7 kg/m2. Table 1. 57.7% of females and 70% of males were obese (BMI > 30 kg/m2); and 58.8% of females and 45% of males had a subjective Epworth sleepiness scale (ESS) value of > 11 points (p > 0.96). Table 2.


141 cases (73.5%) were diagnosed through
RP, and 25.5% through PSG. The mean AHI was
33.1 ± 16.6 in females and 36.5 ± 16 in males
(p > 0.24); and 190 cases (98.9%) presented an
AHI > 15 ev/hour.
The use of the APAP was 3.4 nights ± 1.2 (range
between 2 and 8). 83.8% (163) used the device for 3
nights. Mean compliance with APAP treatment of
the whole population was 373 minutes (6.05 hours ± 1.55), with no gender differences; 380 minutes ± 101 in females and 370 ± 91.2 in males (p > 0.54).
Seventeen patients used full face masks (8.8%)
and minimal contact nasal pillows (3%), whereas
most patients used 14 different models of nasal
masks (88.2%).
Mean pressure values at 90th percentile (P90),
Effp, day 1 Meanp and every day Meanp are detailed
in table 2. Both for males and females, there were
differences regarding the rAHI but not in airway
pressures. Less than 10% of the population presented unacceptability criteria, and the Optt proportion was lower in males (78.9% versus 65.7%) p < 0.001. Table 2.
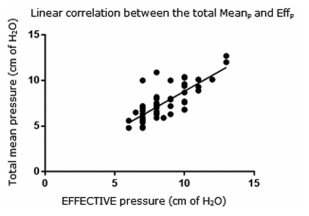
There was a good correlation between the
Meanp and the titration pressure (Effp) that was
finally indicated; r Spearman (rho): 0.73 (95% CI, 0.57-0.84) p < 0.001, y-axis (intercept); 0.1 to -0.1
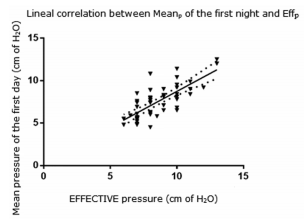
(Figure 1 and 2). In a similar way, the Meanp of
the first night
correlated with the Effp; rho: 0.73
(95% CI, 0.56-0.85) p < 0.001, intercept; 0.2 to -0.3
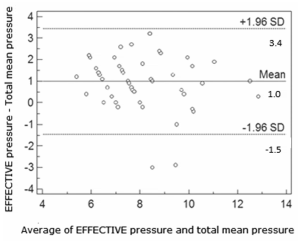
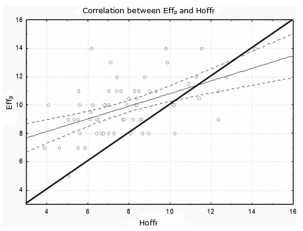
(Figure 3). The Bland and Altman representation
between the Effp and the Hofff showed: intercept:
3.96, β: 0.519 and r2: 0.269 (p < 0.001) (Figure 4).
26% of titrations showed absolute concordance
between both methods, and pressure underestimation by Hofff was frequent, with a negative mean
difference: - 1.98 cm of H2O (95% CI, 1.48-2.49).
The ICC was 0.60 (95% CI: 0.47-0.80) p < 0.0001,
showing a low degree of correlation.
Discussion
Our work summarizes a one year experience of
unsupervised unconventional titrations with autoadjusting CPAP in patients not previously adapted
to the therapy.
This strategy seems to be useful for acquiring
working pressures; it facilitates interface selection
and the initial training of the patient, and makes
it possible to gather data from multiple nights at
the place where the patient usually sleeps with a
low Inadt.
The use of auto-adjustable equipment as a titration method has been validated in the literature
and represents an interesting option18-21, for it
simplifies the procedure and it is not necessary to
make sleep laboratory appointment dates, giving
priority to patients with initial home titration
failure.
We use the visual reading of the pressure/time
and leakage/time chart to define the final Effp value. The values showed by the statistical analysis
derived from the automatic algorithm (P90) used
in this study tend to be higher in bench studies, since the software can´t exclude in the calculation
the moments in which the mask is not adequately
adjusted24. In this case, visual reading can discriminate and exclude pressure values shown under
that circumstance. Also, the Effp is determined
after several nights, excluding periods of no use or
with leakages that imply a not yet corrected rAHI.
We found that 5 to 10 % of APAP titrations have
residual AHIs between 5 and 10 ev/hour with a
greater proportion in males (Table 2). Some definitions consider an acceptable reduction of the AHI
with an APAP of < 10 ev/hour for patients with
OSAHS, though these definitions have not been
evaluated in patients with upper airway resistance
syndrome (UARS) or individuals who remain
sleepy with the use of CPAP25.
Additionally, in our experience, the total Meanp and the Meanp of the first night have a good correlation between themselves and with the Effp (Figures 1 and 3), serving as a guide when there
is great variability of pressures during the night/s.
The rAHI of this kind of devices is reliable information when it is < 10 ev/hour in comparison
with the manual titration by PSG23. However, our
results can´t be extrapolated to other algorithms
since there may be an evident variation in the
performance of each device24.
The influence of the kind of mask on the Meanp and Effp has been previously described. The values
are higher with full face masks, which represented
the minority in our series26. The analysis of our
data shows that careful interface selection and
initial supervision allows ≈ 90% of patients with
no previous experience to use the CPAP > 4 hours
per night with AHI correction.
The compliance figures vary and fluctuate
between 50% and 70%, if a criterion of at least 4
hours/night27-28 is used, although we know that
adherence to the treatment is gradually lost with
time. In the same way, a good initial experience
in the implementation of the treatment is very
important, in such a way that the first CPAP week
is determinant of long-term compliance29-30.
A higher socio-economic level and the increase
in patient age determine a better compliance and
could partly explain the results, since it is an adult
population (≈ 60 years) of a private place21, 32-34 referred to home titration (possible selection bias).
On the other hand, clinical management carried
out by trained personnel and the influence of the
use of cognitive-behavioral strategies can´t be
ignored as a possible incentive to improve shortterm compliance(35-36).
Remarkably, some studies showed that APAP
titration improves mean compliance in approximately one hour, compared to PSG titration at the
sleep laboratory, when compliance was evaluated
three months later37, 38.
On the other hand, the existence of waiting lists
or the delays in the titration have generated predictive formulas based on coefficients according to
anthropometric and functional parameters as the
desaturation index39 or the AHI22, 40. An interesting
study that compared acquired pressures by means
of unsupervised titrations with a different APAP
model (P95 of the Autoset II algorithm) and three
titration formulas, did not find a good correlation
(r2 between 0.66-0.71) and concluded that such
equations must be used carefully41, 42. One strength of our analysis is that we use the Effp of the manual
edition of several nights (finally recommended
pressure) without finding an adequate correlation.
The indices we used (AHI) differ from those of
the PSG (AHI or RDI [respiratory disturbance index]), since in the RP they result from the quotient
between the events and the total recorded time(21,
43, 44), an underestimation factor43, 44 that shall be
taken into account when interpreting the performance of coefficients in the titration formulas.
Conclusions
A high proportion of patients without experience in
the use of CPAP titrate at home with APAP without surveillance and with acceptability criteria.
We did not find an adequate correlation between
the prediction by Hoffstein and Mateika formula
and the effective pressure in our population.
Conflicts of interest: The authors of this work declare there is no conflict of interest related to this publication.
1. Flemons WW, Reiner MA. Measurement properties of the Calgary sleep apnea quality of life. Am J Respir Crit Care Med 2002;165(2):159-64.
2. Peppard PE, Young T, Palta M, Skatrud J. Prospective study of the association between sleep disordered breathing and hypertension. N Engl J Med 2000;342(19):1378-84.
3. Nieto FJ, Young TB, Lind BK, et al. Association of sleep disordered breathing, sleep apnea, and hypertension in a large community-based study. Sleep Heart Health Study. JAMA 2000;283(14);1829-36.
4. Ellen RLB, Marshall SCM, Palayew M, Molnar FJ, Wilson KG, Man-Son-Hing M. Systematic review of motor vehicle crash risk in persons with Sleep Apnea. J Clin Sleep Med. 2006;2(2):193-200.
5. Marin JM, Carrizo SJ, Vicente E, Agusti AG. Long-term cardiovascular outcomes in men with obstructive sleep apnoea-hypopnoea with or without treatment with continuous positive airway pressure: an observational study. Lancet 2005;365(9464):1046-53.
6. National Health and Medical Research Council. Effectiveness of nasal continuous positive airway pressure (CPAP) in obstructive sleep apnea in adults. Endorsered 20 February 2000. En: http://ausinfo.gov.au/general/gen_hottobuy.htm.
7. Morgenthaler TI, Kapen S, Lee-Chiong T, et al. Practice parameters for the medical therapy of obstructive sleep apnea. Standards of Practice Committee of the American Academy of Sleep Medicine. Sleep 2006;29(8):1031-5.
8. Puertas FJ, Pin-Arboledas G, Santa María-Cano J, Durán-Cantolla J. Consenso Nacional sobre el Síndrome de Apneas-Hipopneas del Sueño (SAHS). Grupo Español de Sueño. Arch Bronconeumol 2005;41(S4):72-79.
9. Kushida CA, Littner MR, Morgenthaler T et al. Practice parameters for the indications for polysomnography and related procedures: An update for 2005. Sleep 2005;28(4):499-521.
10. Fernández F, Fernández L, Alberca R. Guía de actuación clínica ante los trastornos del sueño. INSALUD Sociedades Científicas. Vigilia-Sueño 1998;10:14-17.
11. Rey de Castro J, Tagle I, Escalante P. Síndrome de Apnea-Hipopnea Obstructiva del Sueño (SAHOS). Propuesta para su diagnóstico y tratamiento. Comité Apnea Sueño de la Sociedad Peruana de Neumología. Rev Soc Peru Neumología 2001;44:24-8.
12. Obstructive sleep apnea, polysomnography, and splitnight studies: consensus statement of the Connecticut Thoracic Society and the Connecticut Neurological Society. Conn Med 2000;64(8):465-8.
13. McArdle N, Grove A, Devereux G, Mackay-Brown L, Mackay T, Douglas NJ. Split-night versus full-night studies for sleep apnoea/hypopnoea syndrome. Eur Resp J 2000;15(4):670-5.
14. Strollo PJ, Sanders MH, Constantino JP, Walsh SK, Stiller RA, Atwood CW Jr. Split-night studies for the diagnosis and treatment of sleep-disordered breathing. Sleep 1996;19(S10):S255-9.
15. Lloberes P, Ballester E, Montserrat JM, et al. Comparison of manual and automatic CPAP titration in patients with sleep apnea/hypopnea syndrome. Am J Respir Crit Care Med 1996;154:1755-1758.
16. Series F. Accuracy of an unattended home CPAP titration in the treatment of obstructive sleep apnea. Am J Respir Crit Care Med 2000;162(1):94-7.
17. Farré R, Montserrat JM, Rigau J, Trepat X, Pinto P, Navajas D. Response of automatic continuous positive airway pressure devices to different sleep breathing patterns: a bench study. Am J Respir Crit Care Med 2002;166(4):469-73.
18. Montserrat JM, Farre R, Duran J, et al. Performance of an autoCPAP device and its utility used at home for fixed CPAP prescription in OSAS. Eur Respir J 2001;18:515.
19. Montserrat JM, Farre R, Navajas D. Automatic continuous positive airway pressure devices for the treatment of sleep apnea hypopnea syndrome. Sleep Med 2001;2(2):95-8.
20. Morgenthaler TI, Aurora RN, Brown T, Zak R, Alessi C, Boehlecke B, Chesson AL Jr, Friedman L, Kapur V, Maganti R, Owens J, Pancer J, Swick TJ; Standards of Practice Committee of the AASM; American Academy of Sleep Medicine. Practice parameters for the use of autotitrating continuous positive airway pressure devices for titrating pressures and treating adult patients with obstructive sleep apnea syndrome: an update for 2007. An American Academy of Sleep Medicine report. Sleep. 2008 Jan;31(1):141-7.
21. Nogueira F, Nigro C, Cambursano H, Borsini E, Silio J, Avila J (2013). Practical guidelines for the diagnosis and treatment of obstructive sleep apnea syndrome. Medicina (B Aires).;73(4):349-62.
22. Hoffstein V1, Mateika S. Predicting nasal continuous positive airway pressure. Am J Respir Crit Care Med. 1994 Aug;150(2):486-8.
23. Gagmadoux F, Pevernagie D, Jennum P, Lon N, Loiodice C, Tamisier R, van Mierlo P, Trzepizur W, Neddermann M, Machleit A, Jasko J, Pépin JL. Validation of the System One RemStar Auto A-Flex for Obstructive Sleep Apnea Treatment and Detection of Residual Apnea-Hypopnea Index: A European Randomized Trial. J Clin Sleep Med. 2016. Oct 20. Pii: jc-00176-16.
24. Zhu K, Roisman G, Aouf S, Escourrou P. All APAPs Are Not Equivalent for the Treatment of Sleep Disordered Breathing: A Bench Evaluation of Eleven Commercially Available Devices. J Clin Sleep Med. 2015 Jul 15;11(7):725-34.
25. Berry RB, Parish JM, Hartse KM. The use of auto-titrating continuous positive airway pressure for treatment of adult obstructive sleep apnea. An American Academy of Sleep Medicine review. Sleep. 2002 Mar 15;25(2):148-73.
26. Borel JC, Tamisier R, Dias-Domingos S, Sapene M, Martin F, Stach B, Grillet Y, Muir JF, Levy P, Series F, Pepin JL; Scientific Council of The Sleep Registry of the French Federation of Pneumology (OSFP). Type of mask may impact on continuous positive airway pressure adherence in apneic patients. PLoS One. 2013 May 15;8(5):e64382.
27. Kribbs NB, Pack AI, Kline LR, Smith PL, et al. Objective measurement of patterns of nasal CPAP use by patients with obstructive sleep apnea. Am Rev Respir Dis 1993; 147:887-95.
28. Weaver TE, Kribbs NB, Pack AI, et al. Night-to-night variability in CPAP use over the first three months of treatment. Sleep 1997: 20:278-83.
29. Torre-Bouscoulet L, Meza-Vargas MS, Castorena-Maldonado A, Reyes-Zúñeiga M, Pérez-Padilla R. Autoadjusting positive pressure trial in adults with sleep apnea assessed by a simplified diagnostic approach. J Clin Sleep Med. 2008 Aug 15;4(4):341-7.
30. Lewis KE, Seale L, Bartle IE, Watkins AJ, Ebden P. Early predictors of CPAP use for the treatment of OSA. Sleep 2004; 27:134-8.
31. Budhiraja R, Parthasarathy S, Drake CL, et al. Early CPAP use identifies subsequent adherence to CPAP therapy. Sleep 2007; 30:320-4.
32. Giles TL, Lasserson TJ, Smith BH, White J, Wright J, Cates CJ. Continuous positive airways pressure for obstructive sleep apnea in adults. Cochrane Database Syst Rev 2006; 3: CD001106.
33. Grupo español de sueño. Consenso nacional sobre el síndrome de apneas-hipopneas del sueño (SAHS). Arch Bronconeumol 2005; 4: 1-110.
34. Borsini E, Bosio M, Quadrelli S, Villagomez R, Tabaj G, Chertcoff J. Características de acceso al tratamiento con presión positiva en el síndrome de apneas del sueño y su relación con el cumplimiento y el abandono en un hospital de comunidad. Rev Am Med Resp 2010; 1: 4-11.
35. Nogueira JF, Borsini E, Nigro C. Estrategias para mejorar la adaptación al tratamiento con CPAP en pacientes con SAHOS. Rev Am Med Resp 2016; 4: 365-377.
36. Décima T, Maldonado L, Bosio M, Salvado A, Campos J, Quadrelli S, Chertcoff J, Borsini E. Cumplimiento y abandono de la CPAP en pacientes con síndrome de apneas del sueño. Rev Am Med Resp 2013; 4:197-206.
37. Kuna ST, Gurubhagavatula I, Maislin G, Hin S, Hartwig KC, McCloskey S, Hachadoorian R, Hurley S, Gupta R, Staley B, Atwood CW. Noninferiority of functional outcome in ambulatory management of obstructive sleep apnea. Am J Respir Crit Care Med. 2011 May 1;183(9):1238-44.
38. Mulgrew AT, Fox N, Ayas NT, Ryan CF. Diagnosis and initial management of obstructive sleep apnea without polysomnography: a randomized validation study. Ann Intern Med. 2007 Feb 6;146(3):157-66.
39. Stradling JR, Hardinge M, Paxton J, Smith DM. Relative accuracy of algorithm-based prescription of nasal CPAP in OSA. Respir Med. 2004 Feb;98(2):152-4.
40. Sériès F. Accuracy of an unattended home CPAP titration in the treatment of obstructive sleep apnea. Am J Respir Crit Care Med. 2000 Jul;162(1):94-7.
41. Marrone O, Salvaggio A, Romano S, Insalaco G. Automatic titration and calculation by predictive equations for the determination of therapeutic continuous positive airway pressure for obstructive sleep apnea. Chest. 2008 Mar;133(3):670-6.
42. Rodenstein D. Determination of therapeutic continuous positive airway pressure for obstructive sleep apnea using automatic titration: promises not fulfilled. Chest. 2008 Mar;133(3):595-7.
43. Borsini E, Blanco M, Bosio M, Di Tullio F, Ernst G, Salvado A. “Diagnosis of sleep apnea in network” respiratory polygraphy as a decentralization strategy. Sleep Science 9 (2016) 244–248.
44. Berry, R. B., Budhiraja, R, Gottlieb, D.J.et al (2012). Rules for scoring respiratory events in sleep: update of the 2007 AASM Manual for the Scoring of Sleep and Associated Events. Deliberations of the Sleep Apnea Definitions Task Force of the American Academy of Sleep Medicine. J Clin Sleep Med. 8(5):597-619.