Autor : Gallego Claudio, Salomone César, Poropat Alejandra
Hospital General de Agudos Parmenio P. Piñero
Correspondencia : Claudio Walter Gallego cgallego@intramed.net
Abstract
Tuberculosis (TB) has a higher incidence in populations with socio-economic deficits and requires prolonged antibiotic therapy to heal, which hinders adherence to the treatment, with an abandonment rate ranging between 15 and 30% in those with self-administered treatment.
Objectives: to assess the rate of abandonment and to identify predisposing factors in patients monitored at the hospital with self-administered treatment, implemented with weekly controls during the attack phase, and then monthly controls (consolidation phase) until completing the planned schedule.
Materials and methods: all the patients who started treatment between January 1st and December 31st, 2015 were included. A descriptive analysis of the results obtained up to December 31st, 2016 was performed. An interruption ≥ 14 days during the attack phase and ≥ 2 months during the consolidation phase was defined as abandonment by comparing the characteristics of this group with the compliant group using the chi-square test.
Results: 73 patients (38 males) aged 34±15 years were included, 32 were Argentine (44%), and the rest was comprised of: 33 Bolivians, 5 Paraguayans, 2 Peruvians and 1 Chilean. In 47 cases (64%), TB was pulmonary. The extrapulmonary damage included: 11 pleural, 5 nodal, 3 bone (one with a concomitant impact on the psoas and another one on the lung), 2 laryngeal and pulmonary, 2 peritoneal, 2 meningeal and 1 intestinal. In all the cases (except for one that started treatment empirically), the disease was confirmed by direct AFB smear or culture, or by finding granulomas in biopsies performed in a compatible clinical context.
Fifty-two patients completed the treatment (71.2%), 1 patient passed away and 20 abandoned it (27.4%); of the latter, 4 restarted and completed the treatment. The most frequent comorbidities were alcoholism (n = 7), diabetes (n = 6), and HIV positives (n = 6). Compared to the group that completed the treatment, alcoholism was a significant predictive factor for abandonment (2 in 52 vs. 5 in 20; p < .01). There were no significant differences regarding HIV positives (4 in 52 vs. 2 in 20) or gender (9 out of 38 males abandoned treatment vs. 11 out of 34 females). Likewise, there were no differences regarding age, nationality or education level.
Conclusion: with the self-administered treatment system, we obtained an abandonment rate no higher than the expected one at our hospital. Alcoholism was associated with a higher risk of abandonment. Identifying other predisposing factors will help to improve adherence to the treatment by defining specific follow-up strategies.
Key words: Tuberculosis; Treatment compliance; Self-administered treatment.
Introduction
In Argentina, tuberculosis (TB) is associated with high morbimortality1 and it is one of the main public health issues. Epidemiologic monitoring of this disease includes early diagnosis and treatment of the index case as the first measure. This reduces morbimortality and stops transmission to other members of the community2. Concomitantly, the analysis of contacts will enable to extend this strategy by identifying subclinical cases or those cases with latent infections and a higher risk of developing TB in the future, continuing the epidemiological cycle3.
However, the lack of adherence to the treatment of a significant amount of patients compromises these objectives favoring relapses and the development of pharmacological resistance. Many reasons may be associated with the abandonment of treatment. First of all, patients are required to take several antibiotics for a long period of time, which can cause adverse effects as well as a lack of motivation to complete the treatment when the patient becomes asymptomatic. Other factors are linked to the social setting, since this is a disease with an increased incidence in lower-income sectors where factors such as social isolation (lack of family-social support, alcoholism, substance abuse), overcrowding and problems accessing the healthcare system are associated with low adherence4, 5.
To improve compliance with the anti-TB treatment, monitored medication systems were implemented in the seventies under direct observation of healthcare personnel (DOT, Directly Observed Therapy)6. These types of systems, besides consuming more resources, were not categorically successful in decreasing abandonment compared to the self-administered treatment (SAT)7.
The objective of this study is to describe the results from our healthcare center in patients with TB treated with SAT, trying to identify factors associated with lower treatment adherence levels.
Materials and Methods
We included adult patients diagnosed with TB evaluated at a General Hospital of the City of Buenos Aires who had started treatment between January 1st, 2015 and December 31st, 2015, and whose treatment and follow-up was performed entirely at this center. Those who for geographical reasons were referred to other healthcare centers were excluded. The results obtained up to December 31st, 2016 were analyzed.
The treatment schedule implemented was the SAT, with weekly controls during the intensive phase (first 2 months) and then monthly controls until the planned schedule was completed according to national regulations, which take into consideration factors such as organs affected, comorbidities and bacterial resistance to determine the duration of the treatment2.
After completing the follow-up, patients were classified according to:
a) Complete treatment: patient who completed the planned schedule without evidences of treatment failure
b) Treatment failure: patient with TB whose bacilloscopy or sputum culture continues to be positive in or after Month 5 during the treatment.
c) Deceased: patient who died for any reason during the treatment.
d) Abandonment of the treatment: patient who discontinued treatment of TB for ≥ 14 days during the first phase or ≥ 2 months during the consolidation phase
Results are presented as mean ± standard deviation for the numerical variables and as percentages for the categorical variables. A chi-square test was used for the comparisons between groups, considering a p value <0.05 as significant.
Results
Seventy-three patients (38 males, 52%) aged 34±15 years were included. In all the cases (except for one that started treatment empirically), the disease was confirmed by bacilloscopy or positive cultures, or by granulomas in biopsy tissues without other probable causes.
The distribution by nationality was: 32 Argentines (44%) and 33 Bolivians (45%); the rest (11%) included 5 Paraguayans, 2 Peruvians and 1 Chilean.
Table 1 shows the areas affected. In the cases with bone damage, one exhibited a concomitant impact on the psoas muscle and another one on the lung; those with laryngeal damage also had pulmonary lesion.
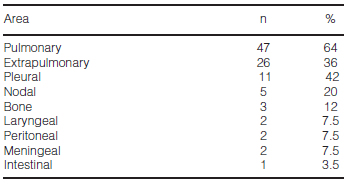

The most frequent comorbidities were: alcoholism (n = 7), diabetes (n = 6), and HIV positives (n = 6). In terms of education level, 33 patients (45%) only had an elementary school level, among whom 1 was illiterate and 9 had not completed elementary school.
Patients were classified based on whether they had completed or abandoned TB treatment, analyzing those factors that could be associated with the lack of adherence to the scheduled treatment (Table 2), excluding from the analysis a deceased case (male, aged 70).
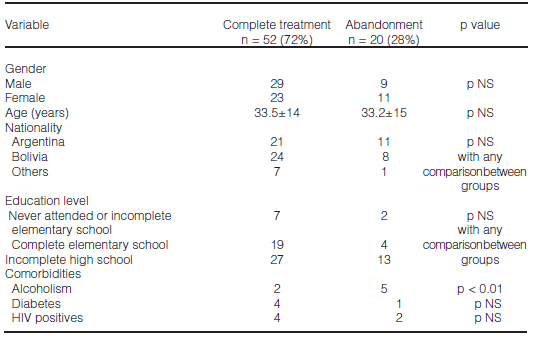
As shown in Table 2, there was no association between treatment abandonment and variables like gender, age, nationality, education level and comorbidities such as diabetes or positive serology for HIV. There was a significant association between alcoholism and abandonment (p = 0.0066). Of all the patients included, 9 had previously undergone a tuberculosis treatment (whether they had completed it or not), and of those only 1 was in the group that abandoned the treatment.
Of the 20 who abandoned, 8 did so during the initial phase of the treatment (first 8 weeks) and the rest during the consolidation phase (between Month 3 and 5). Subsequently, 4 restarted and completed the treatment; therefore, the rate of abandonment and of complete treatments was 21.9% and 76.7%, respectively.
Discussion
This study describes the characteristics of the population with TB assisted at our center, which is linked to a low socio-economic area. Based on statistics of the City of Buenos Aires, the ratio per 100,000 inhabitants corresponding to the assistance area of our hospital is 102, whereas the general rate for the city is 35. Analyzing the nationality of the TB cases reported in 2015, 66% were Argentine for the City of Buenos Aires, whereas 56% were foreign (mostly Bolivians) at our center.
With the SAT strategy developed at our hospital, we obtained 71.2% complete initial treatments, 1 deceased patient and 27.4% abandonments, of which 4 restarted and completed the treatment (final rate of abandonment: 21.9%). Values were similar to those from the last national report (2014)9, which documents 76.7% successful treatments but with a higher mortality rate (7.6% vs. 1.4% found at our center).
In comparison to national statistics, it should be noted that we had a very high percentage of diagnostic confirmation (98.6% vs. 75%), which is probably due to the more extensive diagnostic resources used to obtain samples available at a hospital setting (e.g. fibrobronchoscopy, pleural and extrathoracic biopsies obtained by surgical procedures) and to having a bacterial and anatomopathological laboratory with experience in this disease.
Another factor that determines this difference is that since this is a general hospital, it tends to concentrate extrapulmonary cases (36% vs. 20.5% nationally) in which the accurate diagnosis is actively searched for. In this setting, the most common locations were pleural and nodal, and the rates were similar to the national rates (42% vs. 44% and 19% vs. 20%, respectively).
The rate of complete treatments and abandonments in our population can be considered within the expectations compared to other studies using SAT. At a national level, where DOT was applied in 43% of the cases, the abandonment rate corresponding to 2014 was 16% if considered globally, and 19.4% considering only cases under SAT. However, in said statistic, around 30% of the patients documented did not have a subsequent assessment report, and of these, most (2/3) corresponded to the self-administered treatment. For this reason, there is no sufficient accuracy about the actual rate of patients who abandoned the treatment (the high number of patients without a follow-up can reflect a deficiency in the documentation of abandonments), or about the DOT system having better adherence than the SAT.
A study conducted at another hospital of the City of Buenos Aires10 that compared the DOT vs. the SAT in 1065 patients between 1979-2009, found significant differences when comparing complete treatments and abandonments in both groups (83% vs. 50% and 11.5% vs. 28.6%, respectively). In this study, if patients referred to other centers were excluded from the analysis, the rate of confirmed abandonments would rise up to 33% in the SAT group. On the other hand, the group under SAT had significant differences compared to the DOT, such as a higher rate of previous treatments and of adverse effects; therefore, it seems to be a more vulnerable group where lower adherence to the treatment can be expected, thus justifying increased control.
As to what factors may influence low adherence to the anti-TB treatment, we found that a history of alcoholism is significantly associated with a higher risk of abandonment, which is not the case for gender, nationality, level of education or presence of comorbidities (including HIV+).
One of the limitations of this study is that the number of patients included is low to be able to distinguish the factors linked to a lack of adherence. Various studies describe as social risk factors those associated with social isolation: alcoholism, parenteral drug abuse, prisoners, people without a permanent home, indigents and misfits4, 5, male gender10, 11, lower income11, assistance at a hospital vs. at a Primary Care Health Center11, history of a previous treatment9.
We concluded that with the self-administered treatment implemented at our center, we obtained an abandonment rate no higher than the expected one. Identifying those factors associated with a lack of adherence to the treatment, most frequently present in the population itself, will allow to develop local strategies to optimize compliance, and strategies that are directed toward these specific groups, such as implementing DOTs (if there are resources available to do so) or performing a stricter multidisciplinary follow-up together with social workers.
Acknowledgements: we thank social worker Laura Fernández for her cooperation in this study.
Conflict of interest: The authors declare that there is no conflict of interest associated with this publication.
1. Fernández H, Luque G. Notificación de casos de tuberculosis en la República Argentina. PRO.TB.DOC.TEC.01/16- INER-ANLIS-MSAL
2. Abbate E, Ballester D, Barrera L, et al. Consenso Argentino de Tuberculosis. Rev Arg Med Resp 2009; 9: 61-99.
3. González-Martín J, García-García J, Anibarro L, et al. Documento de consenso sobre diagnóstico, tratamiento y prevención de la tuberculosis. ArchBronconeumol 2010; 46 (5): 255–274.
4. Anibarro L, Lires JA, Iglesias F, Vilariño C, Baloria A, de Lis JM, Ojea R. Factores sociales de riesgo para la falta de cumplimiento terapéutico en pacientes con tuberculosis en Pontevedra. Gac Sanit 2004: 18 (1): 38-44.
5. Arrossi S, Herrero M, Greco A, Ramos S. Factores asociados a la no-adherencia al tratamiento de la tuberculosis: revisión de la literatura. CEDES Área Salud, Economía y Sociedad 2011.
6. Maher D, Chaulet P, Spinaci S, Harries A. Treatment of tuberculosis: guideline for national programmes. 2nd ed. Geneva: WHO 1997.
7. Karumbi J, Garner P. Directly observed therapy for treating tuberculosis. Cochrane Database of Systematic Reviews 2015. Issue 5. Art. No.: CD003343
8. Red de Atención de la Tuberculosis año 2015. Gobierno de la Ciudad de Buenos Aires, 25 de enero de 2016.
9. Armando G, Wettstein M. Resultados del Tratamiento de la cohorte 2014 de casos de tuberculosis en la República Argentina. PRO.TB.DOC.TEC.N°30/16-INER-ANLIS-MSAL
10. González C, Sáenz C, Herrmann E, Jajati M, Kaplan P, Monzón D. Tratamiento directamente observado de la tuberculosis en un hospital de la Ciudad de Buenos Aires. MEDICINA (Buenos Aires) 2012; 72: 371-379.
11. Herrero M, Ramos S, Arrossi S. Determinants of non adherence to tuberculosis tratment in Argentina: barriers related to access to treatment. Rev Bras Epidemiol. 2015 Apr-Jun;18 (2): 287-98.