Autor : Santamaria-Alza Yeison, Romero RondĂ³n Silvia K., SĂ¡nchez Robayo Kelly J., Romero MarĂn MĂ³nica P., Mendoza Herrera Tania, BolĂvar Grimaldos Fabio, TĂ©llez Mosquera Luis E.
Universidad Industrial de Santander, Bucaramanga, Colombia
Correspondencia : Yeison Santamaria Alza yeison-1807@hotmail.com
Abstract
Objective: To determine the variables associated with the development of thoracic fibrocavitary sequelae in patients with a history of pulmonary tuberculosis in Santander.
Methods: A retrospective cohort of 141 patients previously diagnosed with tuberculosis, recruited using non-probability consecutive sampling at pneumology consultations (Hospital Universitario de Santander). A descriptive, bivariate and multivariate analysis was performed with all the variables collected from the medical records.
Results: Sixty-six percent of the patients were males, with an average age of 52+/-16.91 years, evidencing an average time span of 69 months from the moment of the infection to the moment they were recruited, and a history of tobacco use of 46%. Sixty-eight percent stated they had cough and a fibrobronchoscopy was performed in 41%. Eighty-nine percent exhibited some type of sequelae, classified as follows: Parenchymal thoracic 88%, pleural 30%, respiratory tract 45%, mediastinal 38% and vascular 5%. The variables associated with the presence of a sequela were the age of the patient; a period of time exceeding 17 months since the moment of the tuberculosis diagnosis; the age of diagnosis; the diagnostic confirmation of tuberculosis by fibrobronchoscopy and symptoms such as dyspnea, cyanosis and cough.
Discussion: This study establishes the incidence of tuberculosis sequelae in 88.65% of the subjects with tuberculosis treated in Bucaramanga, Santander, Colombia. It is the first study in the region evaluating the factors associated with the development of tuberculosis sequelae, in which the use of fibrobronchoscopies as a diagnostic method was found to be an important factor.
Key words: Pulmonary tuberculosis; Respiratory diseases; Bronchiectases; Remodeling of the airways.
Introduction
Tuberculosis is an infection caused by mycobacterium tuberculosis, an acid-fast bacillus that generates granulomas with central caseous necrosis accompanied by lymphocytes and epithelioid cells. The estimated ratio in Colombia for the year 2014 was 26 cases per 100,000 inhabitants, of which 80.97% corresponded to pulmonary tuberculosis1, 2.
The presence of alterations after treating an episode of tuberculosis is determined as a tuberculosis sequela, provided there is a causal association between it and the reference to a previous infection caused by the bacillus3, 4.
In a study conducted in India, Menon et al. found pulmonary sequelae in 40.36% of the patients under analysis; these were predominantly parenchymal, followed by pleural and mediastinal5.
There are no local studies allowing to determine the risk factors associated with the development of sequelae; however, literature describes the presence of multiresistance6, a history of smoking7 and the lack of treatment or incomplete treatments for tuberculous infections3, 5, 8.
Tuberculosis sequelae can be divided depending on the affected area into parenchymal, of the respiratory tract, pleural, mediastinal and vascular9. Parenchymal sequelae mainly includes caverns, fibrosis and cicatricial atelectases; respiratory tract sequelae mainly includes tracheobronchial stenosis, bronchiectases and bronchopleural or tracheoesophageal fistulas. For pleural sequelae, the most common ones are pleural thickening, pneumothorax, calcified lesions and chronic pleural effusion. Additionally, the most common mediastinal lesions include fibrosis, adenopathies and mediastinal shift. Vascular structures are also affected, with the most relevant sequelae being Rasmussen aneurysms, as well as the thickening and dilation of vascular walls3, 10, 11.
The purpose of this study is to determine the factors associated with the development of thoracic fibrocavitary sequelae in patients with a history of pulmonary tuberculosis in Santander, Colombia.
Materials and Methods
Study design
Observational analytic study using a retrospective cohort with non-probability sampling for concurrent cases of patients under the age of 18 recruited between June 2012 and December 2014 with a history of pulmonary tuberculosis treated at Hospital Universitario de Santander in the city of Bucaramanga, Colombia. With the approval of the medical ethics committee of Instituto Neumológico del Oriente, we collected information from the medical records of patients who attended to pneumology outpatient appointments due to their history of pulmonary tuberculosis, without obtaining their informed consent since the estimated risk was less than minimal.
Patients
We included adult patients previously diagnosed with tuberculosis confirmed by mycobacterial culture, who had completed the treatment established by the national plan for the treatment of tuberculosis, for which the therapy criteria was established through culture and bacilloscopy, with imagenologic records (chest X-ray or CAT scan) corresponding to the conclusion of the follow-up. Patients with pulmonary structural alterations prior to the episode where they became infected with tuberculosis were excluded. The imagenologic report was established as the main outcome of any pulmonary lesion consistent with tuberculosis sequela, described by radiologists from the Radiology and Diagnostic Imaging Department of Hospital Universitario de Santander.
Calculation of the sample size
The calculation of the sample size was performed taking into consideration the incidence rate of tuberculosis in Santander, Colombia in the year 2013 and the prevalence of tuberculosis sequelae reported in literature (40%), with a significance level of 95%, a power of 80% and, in addition, contemplating a 10% loss with a minimum sample size of 130 subjects.
Statistical analysis
The descriptive analysis of the qualitative variables was performed using absolute and relative frequencies. As for the quantitative variables, they are presented as central tendency measures (mean and median) and dispersion measures (standard deviation, interquartile range). A comparison between groups was performed using the Mann- Whitney Test or Fisher’s Test; the association between each of the independent variables and the outcome was evaluated using the chi-square test. Variables with a statistically significant association and p < 0.20 were selected, and a multivariable logistic regression was conducted to find the variables with statistical significance.
Results
Out of 180 prospective patients, 39 did not meet the inclusion criteria; therefore, a total of 141 patients ultimately entered the study. The average age in this cohort was 52+/-16.91 years and 66% were males. When assessing the data associated with the tuberculosis infection episode, we found that the mean age of infection was 46.5 ± 17 years; the mean duration of the treatment was 7.7 ± 4 months and the time elapsed from the moment of the diagnosis to the control by chest imaging was on average 69.3 ± 103.4 months.
The most frequent comorbidities found were pharmacodependence (18%), HIV (15%) and hypertension (13,5%), with a prevalence of active smoking in 46%, exposure to biomass (wood smoke) in 11.3%, cocaine inhalation in 10.6% and passive smoking in 6%. In addition, the reported average age of smoking initiation was between 20.1 ± 9.57 years, with an average daily consumption of 20.23 ± 13 cigarettes and a mean smoking rate of 24.3 ± 31.5 packets/year, as shown in Table 1.
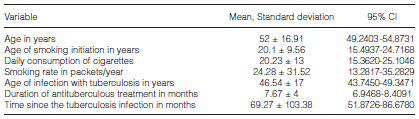
In terms of the drugs used to control the respiratory symptoms, anticholinergics were chronically the most used in 17.7%, followed by the administration of Beta-2 agonists and corticosteroids in 17%, and of oxygen in 2.84%.
The presence of pharmacoresistance was described in 14%, and 24% reported they had previous contact with a patient diagnosed with tuberculosis prior to the infection. In connection with the procedures performed during disease diagnosis or management, the most frequently used ones were fibrobronchoscopies in 41%, lung surgeries in 18% and lung biopsies in 6.38% of the cases. The rate of infectious exacerbations was 27%.
During pneumology outpatient control visits, the most common symptoms reported during the period of treatment were cough (68%), dyspnea (59%), increased sputum and chest pain (32%), and hemoptysis (15.6%); the presence of any imagenologic alteration consistent with a tuberculosis sequela was evaluated, as well as the affected area and the classification according to the described area (parenchymal sequelae, respiratory tract sequelae, mediastinal sequelae, pleural sequelae and vascular sequelae). We reported sequelae in 88.65% of the patients, which were classified according to the affected area into parenchymal sequelae in 79.43%, respiratory tract sequelae in 41.1%, mediastinal sequelae in 34.8%, pleural sequelae in 26.2% and vascular sequelae in 5%, as described in Table 2.
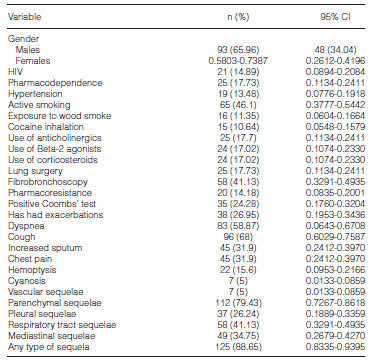
When subgroup analyses were performed, statistically significant differences were found in the distribution of averages in variables such as age, which was higher in patients with sequelae (52.36 years in the group of patients with tuberculosis sequelae and 49.68 in the group of patients without tuberculosis sequelae). A higher rate of males was also found in the group with sequelae (66%) than in the group without sequelae (62%). Likewise, a history of pharmacodependence and smoking; a history of anticholinergic, Beta-2 agonists, inhaled corticosteroids and oxygen use; and a history of lung surgery and fibrobronchoscopy was more common in the group that developed sequelae than in the group that did not. As for the symptoms, dyspnea, cough and hemoptysis had the same pattern. The summary for the analysis of the differences between groups is shown in Table 3.
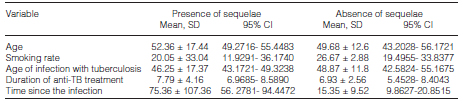
The bivariate analysis was performed taking into account as dependent variable the imagenologic description consistent with tuberculosis sequela and as independent variables the general data, the medical history, the exposure history, the drugs used to control the respiratory symptoms, a history of lung procedures, the data on the tuberculosis infection event and the current symptoms.
Among the variables associated with the risk of having sequelae caused by pulmonary tuberculosis were being over the age of 65 (OR:5.38), having been diagnosed by fibrobronchoscopy during the acute phase (OR:5.68), the use of anticholinergics (OR: 1.16), the use of Beta-2 agonists (OR:1.15), a period of time for the imagenologic diagnostic of the sequela >20 months (OR:9.42), a history of exacerbations (OR:6.3) and the presence of symptoms such as dyspnea (OR:12.88) and cough (OR:4.28); we also found that there were no differences regarding gender and that cyanosis acted as a protective symptom for the presence of sequelae (0.14). (Tabla 4)
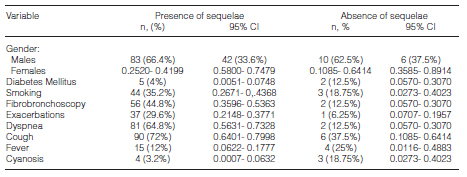
The medical and exposure history evaluated were not statistically significant. Data from the bivariate analysis are shown in Table 5.

A multivariable logistic regression model was implemented using as the outcome variable having sequelae and as independent variables those selected with a p significance level under 0.2 and which evidenced biological plausibility; then, variables with the highest p value were eliminated one by one to obtain the variables that maintained statistical significance in the multivariate analysis.
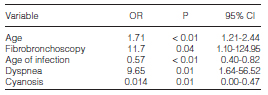
In the multivariate analysis, we obtained a statistically significant association for the presence of tuberculosis sequelae with the following variables: age, performance of a fibrobronchoscopy, age of infection, presence of dyspnea and cyanosis. Data from the multivariate analysis are shown in Table 6.
Discussion
In terms of disease burden, this study establishes a baseline that can be exhibited in one of the countries with the highest rates of tuberculosis, connected to the presence of sequelae after the treatment. It should be noted that, thus far, there was no regional data quantifying the presence of sequelae, which at present are calculated at a rate of 88.65%. This rate is higher than that observed in other countries such as India (43.6%), where it should be emphasized that patients with extrapulmonary tuberculosis (respiratory tract, pleural, mediastinal structures) were also included and a diagnostic classification was permitted with references to bacilloscopies and without positive cultures. These events may have influenced in the outcome due to the likelihood of recruiting false positives.
It is important to highlight the findings of the analysis, which are not part of any previous studies, and which evidenced that older patients, the performance of fibrobronchoscopies and the presence of dyspnea are associated with a statistically significant increase of developing tuberculosis sequelae. By contrast, the younger the patient at the moment of the infection and the presence of cyanosis are associated with a lower risk of developing said alterations.
The association found with the current age of the patient may be explained taking into consideration that the longer the time that has elapsed, the longer the duration of the inflammatory reaction caused by the tuberculosis; thus, the larger the remodeling of the lung structures. A younger age of infection showing a lower risk of developing tuberculosis sequelae may be explained taking into consideration that at a younger age, scarring processes are more precise; therefore, remodeling could be smaller or barely perceptible in chest imaging.
The result associated with fibrobronchoscopies may be explained by the fact that a foreign body is inserted into an inflamed respiratory tract, such is the case of patients with tuberculosis; this can enlarge the lesion during the acute phase, increasing the risk of developing scarring lesions.
Dyspnea in patients with tuberculosis sequelae can be caused by the damage generated to the respiratory tract, which prevents a proper gas exchange and results in the presence of respiratory symptoms, among which the presence of dyspnea is statistically significant. Cyanosis is shown as a variable with a lower risk of developing tuberculosis sequelae. This may be explained by the notion that structural disorders usually do not cause cyanosis; therefore, its presence must be approached by looking for other diseases.
Among the strengths observed in connection with other studies, there is the fact that this is the first study conducted on post-treatment sequelae in a region with a significant level of disease burden, as established by the National Program for the Assistance of Patients with Tuberculosis, which also allows to define a more accurate approach regarding the environment of this population.
Among the limitations, there is the fact that the study does not include the incidence for the entire region due to issues of transhumance, follow-up abandonment and follow-up absence, which should be tackled in the Regional Program for the Management of Anti-tuberculosis. Other important limitations are the potential biases of the study, since its retrospective nature can lead to screening and information biases.
In addition, future studies should include the functional assessment of these patients to determine their medical condition and to complete the data on disease burden exhibited due to tuberculosis sequelae.
Conflict of interest: The authors declare that there is no conflict of interest associated with this publication.
1. Claudia Milena Hormiga Sanchez, Debora Villa Villa, Situacion de la tuberculosis en Santander, 2005-2008, 2009, Revista del Observatorio de Salud Pública de Santander, año 4, numero 3, pp 4-11.
2. Boletín epidemiológico, semana 52, Instituto Nacional de Salud de Colombia, 2014.
3. Machida K, Maekura R. State of the art: sequelae of tuberculosis. Kekkaku. 2005 Oct; 80(10): 655-74.
4. Yoneda R. Tuberculosis sequelae. Kekkaku. 1990 Dec; 65 (12): 827-9.
5. Menon B, Nima G, Dogra V, Jha S. Evaluation of the radiological sequelae after treatment completion in new cases of pulmonary, pleural and mediastinal tuberculosis. Lung India 2015; 32: 241-5.
6. Gayathri Devi, H.J. Complications of Pulmonary Tuberculosis. Department of Pulmonary Medicine, M.S. Ramaiah Medical College, Bangalore, India. 2014.
7. Salkin D, Cadden AV, Edson RC. The natural history of tuberculous tracheobronchitis. Am Rev Tuberc 1943; 47: 351-369.
8. So SY, Lam WK, Yu DYC. Rapid diagnosis of suspected pulmonary tuberculosis by fibreoptic bronchoscopy. Tubercle 1982; 63: 195-200.
9. S-Y. Low, A. Hsu, P. Eng. Interventional bronchoscopy for tuberculous tracheobronchial stenosis. Eur Respir J 2004; 24: 345-347.
10. Hyae K, Koun-Sik S, Jin Go, et al. Thoracic Sequelae and Complications of Tuberculosis. RadioGraphics 2001; 21: 839-860.
11. Seop-eom Jung, Kim Hojoong, Jeon Kyeongman, Um Sang-won, Young-suh Gee, Puo chung Man, et al. Tracheal Wall thickening is associated wiht the granulation tissue formation around silicone stents in patients with post-tuberculosis tracheal stenosis Yonsei Med J, 2013. 54 (4): 949-956.