Autor : Rocco Ana Paula1, Villalba DarĂo1, Feld Viviana1, Leiva Valeria1, Scrigna Mariana1, Distefano Eduardo1, Collins Jessica1, Matesa Amelia1, Rossi Damián1, Areas Laura1, Virgilio Sacha1, Golfarini Nicolás1, Gil Rossetti Gregorio1, Pini MarĂa Paula1, Hannun Marcos1, DĂaz Ballve Pablo2, Buñirigo Pablo1, Noval Diego1, Planells Fernando1
1ClĂnica Basilea, Argentina. 2Hospital Posadas, Argentina
Correspondencia : DarĂo Salvador Villalba e-mail: villalba_dario@yahoo.com.ar
Abstract
Objectives: To describe the incidence of respiratory tract infections (RTIs) in tracheostomized patients hospitalized in a weaning and rehabilitation center (WRC) and to identify risk factors (RFs) for the development of RTI.
Materials and methods: A nested case-control study was conducted. Age was used as the matching variable. All tracheostomized patients who were hospitalized from March, 2013, to February, 2015, were included. The incidence of RTI was recorded.
Results: A total of 167 patients were included, with 73 RTI episodes being recorded in 46 patients (27.5%). Cumulative incidence was 27.5%, and incidence rate was 2.22 episodes per 1,000 days of stay. Bacteria were recovered in 50 of the 73 episodes recorded, with Pseudomonas aeruginosa being the most prevalent organism (34.3%).
The lowest albumin values proved to be a RF for the development of RTI (p 0.001, odds ratio [OR] 5.82, confidence interval [CI] 2.08-16.2). The highest hemoglobin values on admission acted as protective factors (p 0.048, OR 0.74, CI 0.55-0.99). Diagnoses of stroke (p 0.025, OR 3.45, CI 1.16-10.2), Parkinson (p 0.011, OR 18.9, CI 1.93-185) or amyotrophic lateral sclerosis (ALS) (p 0.013, OR 6.34, IC 1.47-27.2) on admission were established as risk factors for the development of RTI.
Conclusion: For the first time in our setting, it was possible to determine the incidence of RTI in tracheostomized patients and the most common pathogens, although comparison with other WRCs is needed. The association found between albumin values and the subsequent development of RTI might be more related to an incidental finding than to a significant clinical difference. Patients with certain neurologic diseases are at increased risk for RTI.
Key words: Respiratory tract infection; Pneumonia; Tracheostomy.
Introduction
Despite advances in antimicrobial therapy and the use of various preventive measures aimed at reducing the incidence of infections, hospital-acquired pneumonia (HAP), ventilator-associated pneumonia (VAP) and healthcare-associated pneumonia (HCAP) lead to increased morbidity and mortality1.
A large body of literature has focused on respiratory tract infections (RTIs) in critically ill patients requiring orotracheal intubation (OTI) hospitalized in intensive care units (ICUs). Little has been reported on the incidence of RTIs in patients who after requiring OTI also receive a tracheostomy (TCT), and existing literature focuses mainly on pediatric populations2, 3. Data on RTIs in adult tracheostomized patients hospitalized in weaning and rehabilitation centers (WRC) are scarce.
Around 10% of patients on assisted mechanical ventilation (AMV) require placement of a TCT4,5. An advantage of performing a TCT is the possibility of referring to a WRC those patients who have recovered from the acute stage of disease and require long-term care and rehabilitation.
Some studies have identified TCT as a risk factor for VAP6-8. A possible explanation for this association could be that tracheostomized patients often require prolonged mechanical ventilation; therefore, the increased incidence of VAP is likely to be related to duration of AMV rather than to TCT itself. In other studies, TCT is described as a protective factor against the development of VAP9.
The present study objectives are to describe the incidence of RTI in tracheostomized patients hospitalized in a WRC and to identify risk factors for the development of RTI.
Materials and methods
An observational prospective cohort study was performed for incidence calculation. A total of 46 cases with RTI were selected from this cohort and matched with 92 controls, and a nested case-control study was carried out. Each case was matched with 2 controls, with age used as the matching variable. The study was conducted at Clínica Basilea, a WRC located in the Autonomous City of Buenos Aires. All tracheostomized patients who were hospitalized from March 1, 2013, to February 28, 2015, were included. Patients younger than 18 years, those requiring emergent TCT to resolve airway obstruction, and those who had a TCT performed to treat head or neck cancer were excluded.
A database was developed to record demographic variables, variables related to ICU hospitalization prior to admission to the WRC, and variables related to WRC hospitalization. Recorded demographic variables included age, gender and past history (cardiovascular, respiratory, neurologic, metabolic and cancer history, smoking status, and long-term home oxygen therapy [HOT] requirement). ICU-related variables were: total length of stay, chief complaint, total days on AMV, and total days of OTI prior to TCT placement. WRC-related variables were: length of stay throughout the study period; development of RTI and number of episodes; maximal inspiratory and expiratory pressures (as measured on admission to the WRC with the use of a one-way valve applied to the TCT cannula), Glasgow Coma Score, creatinine, hemoglobin, albumin, and TSH (WRC admission variables); reason for discharge; and mortality.
Other data recorded were axillary temperature, white blood cell count, change in bronchial secretions (amount, appearance), posteroanterior chest radiograph (lateral if needed), sampling of bronchial secretions in febrile patients (tracheal aspirate and/or bronchoalveolar lavage), AMV requirement (ventilated patient, patient initiating AMV due to the episode, or patient not requiring AMV), type of feeding route (oral, nasogastric tube, or gastrostomy) and whether the patient was being evaluated by swallowing tests (Blue Dye Test by placing blue dye on the patient’s tongue; the test was deemed positive [aspiration] if blue colored secretions were obtained through the TCT cannula and negative if secretions suctioned were not stained with blue dye). The relationship between a positive Blue Dye Test and the onset of the episode (RTI) was recorded if time elapsed between the test and the episode was one week or less.
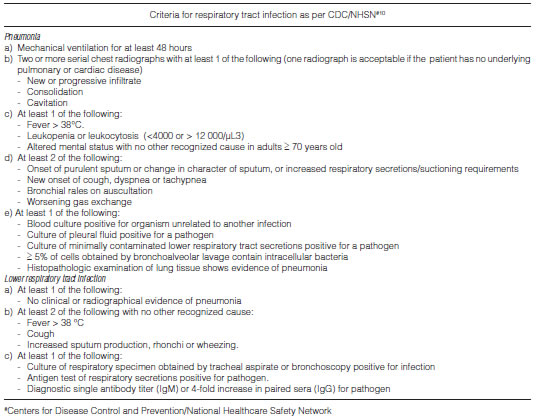
Cumulative incidence and incidence rate of RTI were recorded in the whole study cohort. The incident case of RTI was defined based on criteria established by the Centers for Disease Control and Prevention/National Healthcare Safety Network (CDC/NHSN), which include pneumonia and lower respiratory tract infections (Table 1)10. Overall respiratory infections were recorded, including pneumonia and artificial airway-associated tracheobronchitis, since management in our center is often similar.
Quantitative variables were expressed as mean (X) and standard deviation (±SD) or median (Md) and interquartile range (IQR), according to their distribution, and qualitative variables were presented as absolute frequency and their percentage. The Mann-Whitney test was used to compare continuous variables, and a chi-square test or Fisher’s Exact Test were used for variables measured on a nominal scale, when appropriate. A multivariate binary logistic regression analysis was performed, where presence or absence of RTI was defined as the dependent variable. Factors that could be associated with the development of RTI and having statistical significance (p < 0.1) in univariate comparisons were included in the logistic regression analysis. Wald stepwise elimination method was used, with removal of the variable of less significance at each step to identify factors associated with the development of RTI. An adjustment of the effect measure was performed, with gender and age as confounders. To this end, another multivariate analysis was conducted, where significant variables from the first analysis were included. A Hosmer-Lemeshow test and an area under the curve (AUC) were used to assess calibration and discrimination of the logistic regression model. Statistical significance was set at p ≤ 0.05 for all comparisons.
Results
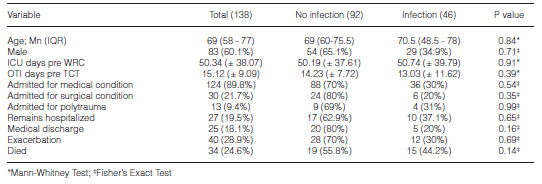
During the study period, 167 patients were included. A total of 73 RTI episodes were recorded in 46 patients, with a cumulative incidence of 27.5%. The incidence rate of RTI was 2.22 episodes/1,000 days of stay in the WRC. Of all patients who developed RTI, 1 had 5 episodes, 1 had 4 episodes, 3 had 3 episodes, 14 had 2 episodes, and the remaining patients had a single episode.
Fifty-three percent of patients with intercurrent RTI were on AMV, 32% were placed on AMV due to the episode, and 15% remained free of AMV.
Feeding was administered through a K 108 nasogastric tube in 59% of patients, through a gastrostomy tube in 36%, and orally in 5%.
Cuff deflation tests were performed within a period of 7 days before the episode of infection in 31.5% of all RTI episodes recorded (23 episodes). Of these, 82% (19 RTI episodes) tested positive on the blue dye test.
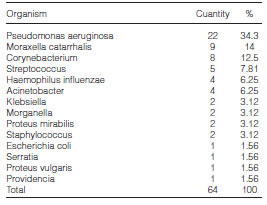
Bacteria were recovered in 50 of the 73 recorded episodes. In 74% of patients in whom bacteria were detected, a single organism was identified; 26% of patients had infections caused by 2 or more organisms. Of all identified organisms (Table 2), Pseudomonas aeruginosa was the most common pathogen (34.3%), followed by Moraxella catarrhalis (14%), and Corynebacterium (12.5%).
In the logistic regression analysis (Table 4), the highest albumin values (p 0.001; OR 0.17; CI 0.06- 0.48) were found to be protective factors against the development of RTI. Similarly, the absence of hypertension and a history of long-term HOT proved to be protective.
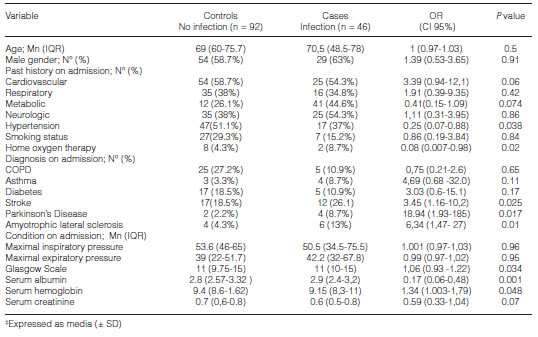
On the other hand, the lowest hemoglobin values on admission to the WRC and the presence of neurologic diseases, such as stroke (p 0.025, OR 3.45 CI 95% 1.16-10.2), ALS (p 0.013, OR 6.34, CI 95% 1.47-27.2), and Parkinson (p 0.011, OR 18.9, CI 95% 1.93-185), proved to be risk factors for the development of RTI.
After adjusting for confounding factors (gender and age), hemoglobin is found to have no statistical significance (p 0.14, OR 0.84, CI 95% 0.67-1.06). (Table 5).
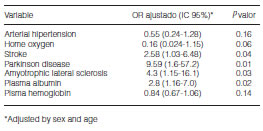
The Hosmer-Lemeshow test to assess calibration of the final binary logistic regression model (with adjustment) showed a p value of 0.93. Discrimination was assessed using the area under the curve, which revealed a value of 0.71.
Discussion
This study is the first in our country to describe respiratory tract infections in tracheostomized patients who are hospitalized in a WRC. The incidence rate and the cumulative incidence of RTI were similar to those reported by Scheinhorn et al.11, who conducted a multicenter study in 1,419 patients receiving prolonged MV admitted to 23 WRC.
In our study, neurologic disease was associated with a risk for developing RTI, which may be related to the swallowing disorders and the impairment of airway protection ability seen in these patients. Nseir et al. also reported an association between neurological impairment and the development of VAP in ICU tracheostomized patients12.
In the present study, patients admitted to our facility were found to have serum albumin levels below normal, similar to the study by Scheinhorn et al.11. The highest albumin values in our sample were associated with a lower risk for development of RTI, a finding consistent with that reported by George et al.13, who found that serum albumin below normal values was a risk factor for the development of infection, which suggests impaired host status, a predisposing factor for infection. Our data, however, show albumin values below reference values in both groups (with and without RTI development), and a difference in medians that has probably no influence on clinical impact, being only a statistical finding.
Other studies conducted at our WRC described the significant difference found in albumin values between the group of patients successfully decannulated and the group with decannulation failure (higher albumin values in the decannulated group)14. As regards successful weaning from AMV, statistically significant differences were found in albumin and hemoglobin values between both groups (higher values in the group weaned from AMV)15.
We did not identify significant differences between cases and controls as regards discharge status from our center. This could be due to the fact that discharge status may depend more on baseline pathology than on RTIs that developed in the WRC. In addition, being this a cohort study, some patients were hospitalized in the WRC before the beginning of the study, and some patients were still hospitalized after the end of the study, making total days of stay analysis difficult. In the study by Scrigna et al.14 on this WRC, the removal of the TCT cannula (decannulation) was found to be one of the determinants of survival and discharge from the WRC.
Only half of patients developing RTIs were on AMV at the time of the episode, which suggests that in this patient group the RTI would be more related to what is known as healthcare-associated pneumonia. However, it is thought that VAP is more related with the presence of an endotracheal tube in the patient’s airway than with the provision of AMV, since the use of noninvasive ventilation reduces the incidence of RTI. In our sample of study patients all have a TCT, but not all require AMV. A small group of patients did not require AMV as a result of the infection.
The relationship between swallow tests and the incidence of RTI could not be analyzed, as during the two-year study period patients in the control group were going through different stages of their swallow tests. However, at the time of the episode of infection, a high proportion of patients were undergoing swallow tests and tested positive for aspiration, which might suggest the possibility of aspiration RTIs.
Of the pathogens recovered by bacteriological examination, Pseudomonas aeruginosa proved to be the most common causative organism, as reported in other studies9, 16. In the multicenter study by Scheinhorn, the most commonly reported organism was Staphylococcus aureus11, which reflects the fact that each institution has its own local microbial flora.
One limitation of our study is its retrospective design; however, data were prospectively collected. In addition, as this was a single center study, our results cannot be extrapolated to other WRCs. Moreover, since some patients who are successfully weaned from AMV later require reintubation, we were unable to record AMV duration for each patient at the time of the episode and total days of AMV during the study period. Also, we did not consider antimicrobial therapy given before the episode.
Conclusion
For the first time in our setting, the incidence of RTIs in tracheostomized patients and the most common causative agents were determined, although our results should be contrasted with those of other WRC. The association found between albumin values and the subsequent development of RTI may be more related to an incidental finding than to a significant clinical difference. Patients with certain diagnoses of neurologic disease have a higher risk for RTI.
References
1. American Thoracic Society; Infectious Diseases Society of America. Guidelines for the management of adults with hospital-acquired, ventilator-associated and healthcare-associated pneumonia. Am J Respir Crit Care Med. 2005; 171(49): 388-416.
2. Barret JP, Desai MH, Herndon DN. Effects of tracheostomies on infection and airway complications in pediatric burn patients. Burns. 2000; 26(2): 190-3.
3. Hsia SH, Lin JJ, Huang IA, Wu CT. Outcome of long-term mechanical ventilation support in children. Pediatr Neonatol. 2012; 53(5): 304-8.
4. Kollef MH, Ahrens TS, Shannon W. Clinical predictors and outcomes for patients requiring tracheostomy in the intensive care unit. Crit Care Med. 1999; 27: 1714-20.
5. Fischler L, Erhart S, Kleger GR, Frutiger A. Prevalence of tracheostomy in ICU patients: a nation-wide survey in Switzerland. Intensive Care Med. 2000; 26: 1428-33.
6. Celis R, Torres A, Gatell J, et al. Nosocomial pneumonia: a multivariate analysis of risk and prognosis. Chest 1988; 93: 318-324.
7. Torres A, Aznar R, Gatell JM, et al. Incidence, risk and prognosis factors of nosocomial pneumonia in mechanically ventilated patients. Am Rev Respir Dis 1990; 142: 523-8.
8. Kollef MH, Von Harz B, Prentice D, et al. Patient transport from intensive care increases the risk of developing ventilator-associated pneumonia. Chest 1997; 112: 765-773.
9. Lou Sole, Talbert S, Aragon Penoyer D, Bennett M, Sokol S, Wilson J. Comparison of respiratory infections before and after percutaneous tracheostomy. Am J Crit Care 2014 Nov; 23(6): e80-7.
10. Horan TC, Andrus M, Dudeck MA. CDC/NHSN surveillance definition of health care-associated infection and criteria for specific types of infections in the acute care setting. Am J Infect Control. 2008; 36(5): 309-332.
11. Scheinhorn DJ, Hassenpflug MS, Votto JJ, et al. Post-ICU Mechanical Ventilation at 23 Long-term Care Hospitals. A Multicenter Outcomes Study. Chest. 2007; 131: 85-93.
12. Nseir S, Di Pompeo C, Jozefowicz E, et al. Relationship between tracheotomy and ventilator-associated pneumonia: a case-control study Eur Respir J. 2007; 30: 314-320.
13. George D, Falk P, Wunderink R, et al. Epidemiology of ventilator-acquired pneumonia based on protected bronchoscopic sampling. Am J Respir Crit Care Med. 1998; 158: 1839-1847.
14. Scrigna M, Plotnikow G, Feld V, et al. Decannulation after the ICU Stay. Analysis of 181 Tracheostomized Patients. Rev Am Med Resp 2013; 2: 58-63.
15. Villalba D, Plotnikow G, Feld V, Rivero Vairo N, Scapellato J, Díaz Nielsen E. Weaning from prolonged mechanical ventilation at 72 hours of spontaneous breathing. MEDICINA (Buenos Aires) 2015; 75: 11-7.
16. Ahmed QA, Niederman MS. Respiratory infection in the chronically critically ill patient. Ventilator-associated pneumonia and tracheobronchitis. Clin Chest Med. 2001 Mar; 22(1): 71-85.