Autor : Julia Vasquez1, 2, Juan Ossés1, 2, Jorge Cáneva1, 2, Juana Ahumada1, 2, Graciela Wagner1, 2, Carmen Gómez2, Roberto Favaloro2, Alejandro Bertolotti2
1 Pulmonology Service. Hospital Universitario Fundación Favaloro. Buenos Aires. Argentina. 2 Intrathoracic Transplantation Division. Hospital Universitario Fundación Favaloro. Buenos Aires. Argentina
Correspondencia : Julia Vasquez Mailing address: Av Belgrano 1782, 3rd foor, 1093 - CABA Telephone number: 43781200/1300, extension number: 3380/85 Fax number: 43781200, extension number: 3390. E-mail: julia75_vasquez@hotmail.com
Abstract
Introduction and objectives: Emphysema is the most frequent indication for lung
transplant (LT). The purpose of this study was to assess demographic and functional
characteristics of patients with emphysema and analyze survival.
Methods: Analytic observational study conducted in 84 patients with emphysema who
received a LT between June 1994 and March 2012. Survival was analyzed with the
Kaplan-Meier method.
Results: 84 LTs were performed in 84 patients with chronic obstructive pulmonary disease (COPD) due to advanced emphysema. All the patients were smokers; 11 patients
(13%) showed alpha 1-antitrypsin deficiency (A1AD); 70 out of 84 transplants (83%)
were single-lung transplants (SLT) and 14 (17%) were double-lung transplants (DLT);
69 (82%) were elective transplants and 15 (18%) were emergency/urgency transplants.
Mean age: 54.95 ± 6.10 years, 54 male (64%). Forced expiratory volume in first second
(FEV1): 0.60 ± 0.28 l (20 ± 9%); forced vital capacity (FVC): 1.78 ± 0.62 l (46 ± 16%);
mean pulmonary arterial pressure (MPAP): 21.08 ± 5.79 mmHg; partial pressure of arterial
oxygen (PaO2): 67.54 ± 12.27 mmHg; partial pressure of arterial carbon dioxide (PaCO2):
46.40 ± 8.04 mmHg; six minute walk test (6MWT) distance: 225.59 ± 113.67 m; hospital
mortality (HM): 16% (13/84); overall survival at 1, 3, 5, 7 and 10 years: 67%, 53%, 40%,
27% and 13%; conditional survival at 3, 5, 7 and 10 years: 79%, 59%, 41% and 20%.
Conclusions: LT is a therapeutic option for advanced emphysema. This study shows the
characteristics and survival of COPD patients who underwent lung transplantation at the
Hospital Universitario Fundación Favaloro (HUFF).
Key words: Lung transplantation; Emphysema; COPD
Introduction
COPD is characterized by the presence of chronic
and partially reversible airflow obstruction, secondary to an anomalous inflammatory reaction
mainly to tobacco smoke, even though only one
fourth of smokers develop COPD1.
Homozygous A1AD is associated with early
emphysema in smokers2 and represents approximately 2% of cases of emphysema.
Referral of patients with COPD for LT shall
be considered if there is evidence of progressive
impairment, despite an optimum treatment with
bronchodilators, oxygen and respiratory rehabilitation. It is complicated to determine the suitable
moment to make the referral, since patients with
COPD may have a relatively good prognosis for
survival3 in spite of the fact that they are very
symptomatic and limited.
Recent data suggest a survival improvement in
patients with COPD who underwent LT, in comparison with other diagnoses4.
As indicated in the international guides for the
selection of LT candidates, the transplant shall be
performed when post-transplant life expectancy is
higher than life expectancy without the procedure5, 6.
Median survival after LT in patients with COPD
is approximately 5 years7.
According to the 2010 regulation of the Unique
Central National Institute Coordinator of Ablation
and Transplant (INCUCAI), there are different
clinical situations for lung transplantation (single
or double-lung) and heart-lung transplantation.
• Emergency: Patients at the critical care unit
(coronary care unit [CCU] or intensive care unit
[ICU]), that meet one of the following criteria:
– Intubated patients receiving mechanical
respiratory assistance
– ECMO (extracorporeal membrane oxygenation)
– Diagnosis of pulmonary fibrosis, cystic fibrosis or bronchiectases plus
• NIV (noninvasive ventilation)
– Diagnosis of primary pulmonary vascular
disease plus
• Functional class (FC) IV according to the
New York Heart Association (NYHA) functional classification, in need of inotropes
and/or vasodilators plus:
• Pericardial effusion or
• Serious impairment of the RVSF (right
ventricular systolic function) by echocardiogram or RA (right atrium) mean pressure ≥ 20 mm
• Emergency A: Patients at the critical care unit
(CCU/ICU/intermediate care unit), that meet
one of the following criteria:
– FC IV cystic fibrosis or pulmonary fibrosis
plus:
• Systolic pulmonary artery pressure ≥ 70
mmHg or
• Hypercapnia ≥ 70 mmHg
– COPD with NIV
– FC IV primary pulmonary vascular disease
with maximum vasodilator therapy including
prostanoids
• Emergency B: Outpatient recipients that meet
the following criteria:
– NIV
– Intravenous, subcutaneous or inhalatory
vasodilator therapy with prostanoids
Patients who underwent LT showed an improved pulmonary function8, 9 and a better quality
of life10, 11.
Despite improvements in the preservation of
the pulmonary graft12 and postoperative care,
the incidence of complications and morbidity and
mortality of this type of transplant is still considerable13, 14.
According to the data of the international registry
of the International Society for Heart and Lung Transplantation (ISHLT) published in 201115, emphysema
is the most frequent indication for SLT or DLT.
The analysis of this series is based on the ISHTL
2006 consensus that was in force when this study
was developed.
New ISHLT criteria that have been recently
published update referral and transplant criteria
for patients with advanced pulmonary disease16.
The objectives of this study intend to know the
demographic and functional characteristics and
survival of patients with COPD due to advanced
emphysema who received a LT at the HUFF.
Patients and Methods
An analytic and observational study was performed with retrospective data collection from patients diagnosed with advanced emphysema who
received a LT in the HUFF between June 1994
(when the LT program began) and March 2012.
Follow-up of the recipients included in this study
was performed until their death or until the end
of the study on March 31, 2012.
The diagnostic criteria for emphysema are based
on the medical record, computed tomography and
respiratory function tests.
Variables were collected from 84 patients who
were consecutively transplanted. Pretransplant
demographic and clinical characteristics, immediate postoperative evolution and long-term survival
were retrospectively analyzed. This information
was obtained from the database of the HUFF LT
team and medical records.
All the patients signed an informed consent before
admission for LT or treatment of transplant complications. The informed consent included the surgical
treatment they would undergo, its complications and
data management, since it was a university hospital.
The analyzed variables were: age, gender, FEV1;
FVC; MPAP; PaO2; PaCO2, 6MWT total distance,
HM, overall survival and conditional survival.
Demographic Variables
Gender: Either male or female.
Age: The age of the patient when the LT was
performed, expressed in years.
Functional Variables: At the time of the
study for inclusion in the lung transplantation
waiting list (LTWL).
FVC: Expressed as an absolute value in liters
(l), and also as a percentage of the corresponding
aforementioned theoretical values according to
age, gender, height and race.
FEV1: Expressed as an absolute value in liters
(l), and also as a percentage of the corresponding
aforementioned theoretical values according to
age, gender, height and race.
PaO2: Partial pressure of O2 in baseline arterial blood at ambient air, measured before the LT,
expressed in mmHg.
PaCO2: Partial pressure of CO2 in baseline arterial blood at ambient air, measured before the LT,
expressed in mmHg.
6MWT: The total distance was calculated, expressed in m.
Main Hemodynamic Variable
MPAP: Mean pulmonary arterial pressure measured by right cardiac catheterization and expressed in mmHg.
Survival
Hospital Mortality: The mortality that was
recorded within the first 30 days after the LT, expressed as an absolute number and a percentage
of the total amount of transplant patients.
Overall Survival: The possibility to survive
beyond certain amount of time (expressed in
years). It was calculated taking into account the
time from the LT until the death of the patient or
end of study.
Conditional Survival: The possibility to survive beyond certain amount of time (expressed in
years), excluding the first year after the transplant.
It was calculated taking into account the time from
the LT until the death of the patient or end of
study, only in the case of patients whose survival
times were greater than one year.
Statistical Analysis
The patients of the study were subjected to a
descriptive analysis. The results of continuous
variables are expressed by means of average and
standard deviation (SD), whereas categorical
variables are expressed by means of percentage,
absolute and relative frequencies.
The survival experience of transplant patients
was determined by calculating the curves with
the Kaplan-Meier method, and the comparison
between groups (defined by the clinical status of the patients and the type of pulmonary transplant
that was performed) was made by the Log-Rank
Test. Hospital mortality was particularly analyzed
(within the first month after surgery).
An associated probability (p) ≤ 0.05 was considered as statistically significant.
The survival analysis, including the charts, was
made with SAS software, version 9.2.
Results
During the study period, 84 consecutive de novo
LTs were performed in 84 patients due to emphysema.
11 of the 84 de novo LTs (13%) had A1AD.
70 SLTs (83%) and 14 DLTs (17%) were performed; 69 (82%) were elective transplants and 15
(18%) were emergency/urgency transplants. Mean
age was 54.95 ± 6.10 years; 54 patients (64%) were
male. Functional and hemodynamic characteristics
at the time of the evaluation for inclusion in the
waiting list were as follows: FEV1: 0.60 ± 0.28 l
(20 ± 9% of the aforementioned value); FVC: 1.78 ± 0.62 l (46 ± 16% of the aforementioned value);
MPAP: 21.08 ± 5.79 mmHg; PaO2: 67.54 ± 12.27
mmHg; PaCO2: 46.40 ± 8.04 mmHg; 6MWTD
distance: 225.59 ± 113.67 m (Tables 1, 2, 3 and 4).
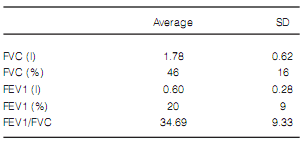
FVC: Forced vital capacity; l: liters; FEV1: Forced expiratory volume in first second
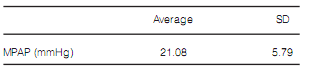
MPAP: Mean pulmonary arterial pressure; SD: Standard deviation

PaO2: Partial pressure of oxygen in arterial blood; PaCO2: Partial pressure of carbon dioxide in arterial blood; SD: Standard deviation
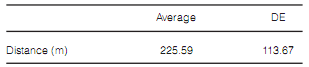
SD: Standard deviation
At the end of this study, 35% of patients (29)
were alive and the remaining 66% (55) had died.
The available follow-up was 248.7 patient-years.
Hospital mortality (30 days) was 13/84 (16%).
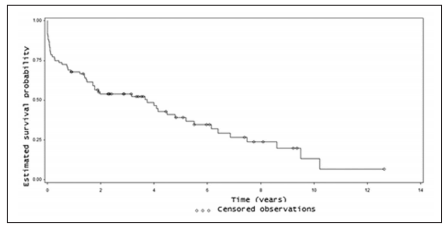
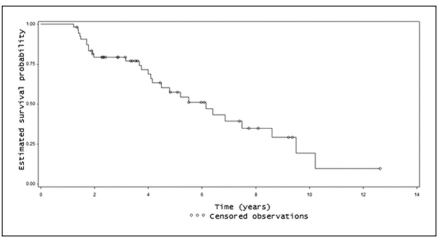
Estimated overall survival after 1, 3, 5, 7 and
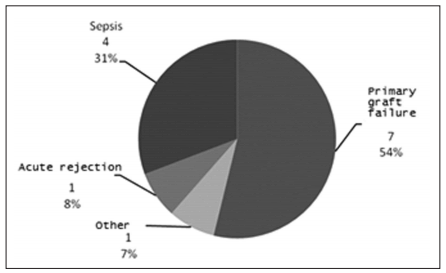
10 years was 67%, 53%, 40%, 27% and 13%, respectively (Figure 1). The main cause of hospital
mortality was primary graft failure (54%) (Figure
2). Excluding the first year post-transplantation
(conditional survival), the survival after 3, 5, 7 and
10 years was 79%, 59%, 41% and 20% (Figure 3).
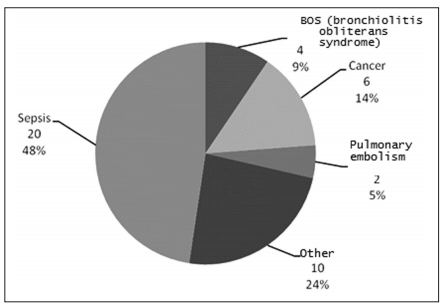
At follow-up, sepsis was the most frequent cause
of mortality (48%) (Figure 4).
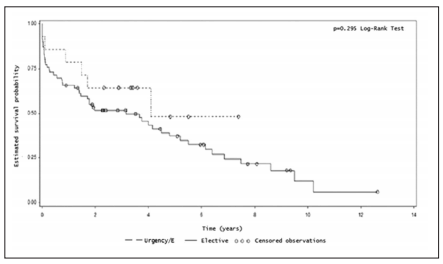
No differences were found in the overall survival of the patients regarding their clinical status, elective versus emergency/urgency. Estimated survival after one year was 66% for the first group and 71% for the second group (p=0.295, Log-Rank Test) (Figure 5). No differences were found in the overall survival of the patients regarding the type of transplant, single-lung versus double-lung (p= 0.560, Log-Rank Test) (Figure 6).
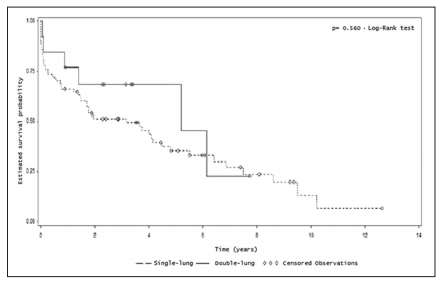
These results may be a consequence of the fact that the DLT population was not as large as the SLT population.
Discussion
COPD is the most frequent indication for LT, both
on the international and national levels. The 2011
ISHLT registry established that 36% of transplant
patients were transplanted due to advanced pulmonary emphysema. The percentage increases
to 43% if we include patients with emphysema
secondary to A1AD15.
On an institutional level, COPD is also the most
frequent indication for LT. In our global series, approximately 40% of patients who have undergone
LT had COPD. Significant male predominance
was confirmed within LT recipients due to COPD
(64%). However, when reviewing the North American series, these data are surprisingly reversed,
as with Cassivi et al17, where almost two thirds
of the 306 patients (60.5%) were females. These
differences could be explained by the different
smoking habits between males and females in the
countries under study.
The mean age of the patients of our series, 54.95
years, is similar to that of the Cassivi et al work,
55 years17, and to other international groups18.
In our series, the percentage of patients affected
by A1AD was 14%. According to the consulted
literature, it is a very variable percentage: 6% obtained at the ISHLT15 international registry, 28%
at the Cassivi et al17 work, 27.4% published by Delgado et al19 and 32.9% at the Burton et al20 work.
Regarding the breathing functional condition of
the patients, the results of the spirometry performed before the LT show highly developed conditions, with mean FEV1 values of 0.60 l (20% of the
reference value) similar to those reported by other
authors17,18, 21, 22. The exercise tolerance of patients
the moment they were included in the LTWL also
decreased considerably, with an average of 225.59
m at the 6MWT; these results are similar to other
studies17, 21, 22. Such a considerable involvement of
the breathing reserve and exercise capacity is one
of the main indications for this kind of patients to
be included in a LT program.
Regarding the kind of procedure, we should
emphasize the predominance of SLTs, which represent 83% of LTs performed in our group during
the period under study.
These data are within a range that very much
differs from that offered by the 2011 ISHLT international registry15, where DLTs predominate
(approximately 70%) in COPD patients.
However, if we analyze the related literature
individually, we can observe certain disparity in
the data. The results revealed by Cassivi et al17 or
Lahzami et al23 are similar to the results reported
by the ISHLT in 2011, with a double-lung procedure rate of 67% and 65%, respectively. However, in
other international groups, such as Staven et al or
Gunes et al18, there are fewer double-lung procedures in COPD patients: 43% and 38%, respectively.
On the local level, initial data derive from a collaborative group that was created for the purpose
of implementing a LT joint program. Between June
1993 and February 1996, 6 right lung SLTs and 1
sequential DLT were performed in 7 patients with
chronic respiratory insufficiency due to pulmonary
emphysema associated with a smoking habit24.
Some years later, a longer-term publication revealed the following related data: between October
1990 and March 2003, 79 LTs were performed: 25
heart-lung transplants (31.6%), 36 SLTs (45.5%)
and 18 DLTs (22.7%). The SLTs began in June
1994, and the DLTs in 1996. Indications for SLT
(n = 36) were emphysema (n = 23) and pulmonary
fibrosis (n = 13). Indications for DLT (n = 18) were
secondary bronchiectases (n = 8), cystic fibrosis
(n = 8), pulmonary emphysema (n = 1) and bronchiolitis obliterans caused by graft-versus-host
disease after a bone marrow transplant (n = 1).
Excluding heart-lung transplants, there was a
total of 54 LTs, including SLTs and DLTs, 44.4%
of which (n = 24) were due to emphysema. 96%
of the emphysema cases were SLTs (n = 23) and
4% were DLTs (n = 1)25. In both national studies,
there was a predominance of SLTs.
Patients with emphysema may receive a SLT
or a DLT, since the differences observed in the
post-surgery exercise capacity and quality of life
are irrelevant15.
Indication for SLT in patients with emphysema was controversial in the mid 80s, since it
was considered highly probable that as a result
of the transplant, perfusion would be preferably
distributed in the grafted lung (due to its lower
vascular resistance), and most of the ventilation
would reach the native lung (as a consequence of
greater compliance), possibly generating a serious
ventilation-perfusion mismatch. Also, the native
emphysematous lung could hyperinflate even
more, displace the mediastinum and compress the
transplanted lung. Although it has been observed
in the practice that the native lung keeps hyperinflating after the transplant, various groups have
revealed excellent functional results in emphysematous patients with SLT24.
The ISHLT reported in 2002 that patients with
bilateral transplants had better survival rates.
However, with the SLT, a greater number of patients in the waiting list26 can be transplanted.
The LT procedure in COPD patients has a hig rate of morbidity and mortality after surgery27. In
our surgery, HM was established at 16%. These
data differ greatly from the data revealed by Günes
et al18, where in a cohort study of 173 transplanted
patients with COPD, there was 95% survival after
30 days, implying a HM of only 5%.
However, it is complicated to make a comparison between most of the authors who analyze
this parameter, since there´s no uniformity in the
time period under analysis or in the subsequent
publication of this information.
Cassivi et al17 reveal similar data, with a really
low HM of 6.2%, in one of the longest series that
were published in this regard, even though they
do not define the exact time period.
The patients of our series had 40% probability of
five-year overall survival. These results are slightly
lower than the data published in the 2011 ISHLT
report, where the five-year survival rate for COPD
patients was established around 50%15.
Most published series establish a five-year survival rate of approximately 60%17, 20, 26,30.
When analyzing conditional survival after the
first year, as revealed in the annual ISHLT report26,
we got a five-year survival rate of 59%, similar to
that published in previous ISHLT reports15, 28, 29,31 which was established around 60%. LT profitability in patients diagnosed with COPD, in terms of
survival, is still a controversial issue, as shown in
the recent publication of various articles and reviews in this regard32-35, due to the fact that there
are different studies in favor36-39 and against6 LT
with this indication.
Our results reveal that patients who received a
SLT did not show a greater death risk than DLT
recipients.
The survival of LT patients reported in recent
years shows better results due to the optimization
of immunosuppressive therapy and control of
infectious complications. Also, in recent years we
observed an increase in the number of patients
with urgency/emergency transplants. Despite the
fact that there is a greater risk within this population, this trend did not modify hospital or overall
mortality in a significant way.
Conclusion
LT in COPD patients is a therapeutic option for subjects with advanced emphysema who meet the criteria for lung transplantation. Also, the results of the five-year overall survival analysis carried out in our institution were lower than the results of the reports published by the ISHLT, but can be considered similar if we take into account the five-year conditional survival.
Conflicts of Interest: AB received funding from Gador SA, Novartis and Roche to attend transplant congresses; as a medical advisor to Thoratec, in mechanical circulatory support, he has informed the media about donation and organ transplantation, with the institutional interest of the Hospital Universitario Fundación Favaloro. JC received funding from GlaxoSmithKline and Bayer to attend congresses; he is main investigator of clinical trials on pulmonary hipertension funded by Actelion and Bayer.
1. Fletcher C, Peto R. The natural history of chronic airflow obstruction. Br Med J 1977; 1:1645-8.
2. Alpha-1-Antitrypsin Deficiency Registry Study Group. Survival and FEV1 decline in individuals with severe deficiency of alpha1- antitrypsin.Am J Respir Crit Care Med 1998; 158: 49-59.
3. Orens JB, Estenne M, Arcasoy S et al. International guidelines for the selection of lung transplant candidates: 2006 update. A consensus report from the PulmonaryScientific Council of the International Society for Heart and Lung Transplantation. J Heart Lung Transplant 2006; 25: 745-55.
4. Martínez FJ, Kotloff R. Prognostication in Chronic Obstructive Pulmonary Disease: implications for lung transplantation. Semin Respir Crit Care Med 2001; 22: 489-98.
5. American Society for Transplant Physicians; American Thoracic Society; European Respiratory Society; International Society for Heart and Lung Transplantation. International guidelines for the selection of lung transplant candidates. Am J Respir Crit Care Med 1998; 158: 335-39.
6. Stavem K, Bjortuft O, Borgan O, Geiran O, Boe J. Lung transplantation in patients with chronic obstructive pulmonary disease in a national cohort is without obvious survival beneft. J Heart Lung Transplant 2006; 25: 75-84.
7. Hertz MI, Boucek MM, Edwards LB et al. The ISHLT transplant registry: moving forward. J Heart Lung Transplant 2006; 25: 1179-85.
8. Trulock EP. Lung transplantation. Am J Respir Crit Care Med 1997; 155:789-818.
9. Grossman RF, Frost A, Zamel N et al. Results of single lung transplantation for bilateral pulmonary fibrosis. The Toronto Lung Transplant Group. N Engl J Med 1990; 322: 727-33.
10. TenVergert EM, Essink-Bot ML, Geertsma A et al. The effect of lung transplantation on health-related quality of life: a longitudinal study. Chest 1998; 113: 358-64.
11. MacNaughton KL, Rodrigue JR, Cicale M, Staples EM. Health-related quality of life and symptom frequency before and after lung transplantation. Clin Transplant 1998; 12: 320-3.
12. Miñambres E, González-Castro A, Rabanal JM et al. Comparative study of two preservation solutions in the initial function after bilateral human lung transplantation. Med Intensiva 2007; 31:1-5.
13. González-Castro A, Suberviola B, Llorca J, González-Mansilla C, Ortiz-Melón F, Miñambres E. Prognosis factors in lung transplant recipients readmitted to the intensive care unit. Transplant Proc 2007; 39: 2420-1.
14. González-Castro A, Llorca J, Burón J, Suberviola B, Vallejo A, Miñambres E. Evaluation of the oxygenation ratio as long-term prognostic marker after lung transplantation. Transplant Proc2007; 39: 2422–4
15. Christie JD, Edwards LB, Kucheryavaya AY et al. The Registry of the International Society for Heart and Lung Transplantation: Twenty-eighth Adult Lung and Heart-Lung Transplant Report-2011. J Heart Lung Transplant 2011; 30: 1104-22.
16. Weill D, Benden C, Corris P et al. A consensus document for the selection of lung transplant candidates: 2014-An update from the Pulmonary Transplantation Council of the International Society for Heart and Lung Transplantation. The Journal of Heart and Lung Transplantation 2015; 34: 1-15.
17. Cassivi SD, Meyers BF, Battafarano RJ et al. Thirteen-year experience in lung transplantation for emphysema. Ann Thorac Surg 2002; 74: 1663-9.
18. Gunes A, Aboyoun CL, Morton JM, Plit M, Malouf MA, Glanville AR. Lung transplantation for chronic obstructive pulmonary disease at St Vincent’s Hospital. Intern Med J 2006; 36 : 5-11.
19. Delgado M, Borro JM, De La Torre MM et al. Lung transplantation as the first choice in emphysema. Transplant Proc 2009; 41:2207-9.
20. Burton CM, Milman N, Carlsen J et al. The Copenhagen National Lung Transplant Group: survival after single lung, double lung, and heart-lung transplantation. J Heart Lung Transplant 2005; 24: 1834-43.
21. Ferrer J, Rodríguez E, Román A et al.Factors related to postoperative mortality in lung transplantation for emphysema. Transplant Proc 2007; 39: 3317-22.
22. Miñambres E, Zurbano F, Naranjo S, Llorca J, Cifrián JM, González-Castro A. Trasplante de pulmón en casos de enfisema: análisis de la mortalidad. Arch Bronconeumol 2009; 45: 335-40.
23. Lahzami S, Bridevaux PO, Soccal PM et al. Survival impact of lung transplantation for COPD. Eur Respir J 2010; 36: 74-80.
24. Grupo Cooperativo Fundación Favaloro- Hospital María Ferrer. Trasplante de pulmón en enfisema. Medicina1997; 57: 521-29.
25. Favaloro R, Bertolotti A, Gómez C et al. Lung Transplant at the Favaloro Foundation: A 13-Year Experience. Transplantation Proceedings 2004; 36 : 1689-91
26. Thabut G, Christie JD, Ravaud P et al. Survival after bilateral versus single lung transplantation for patients with chronic obstructive pulmonary disease: a retrospective analysis of registry data. Lancet 2008; 371: 744-51.
27. Cerón Navarro J, Aguiar Quevedo K, Mancheño Franch N et al. Complicaciones del trasplante de pulmón en la enfermedad pulmonar obstructiva crónica. Medicina Clinica (Barc) 2013; 140:385–89.
28. Christie JD, Edwards LB, Kucheryavaya AY et al. The Registry of the International Society for Heart and Lung Transplantation: twenty-seventh official adult lung and heart-lung transplant report-2010. J HeartLung Transplant 2010; 29: 1104-18.
29. Christie JD, Edwards LB, Aurora P et al. Registry of the International Society for Heart and Lung Transplantation: twenty-fifth official adult lung and heart/lung transplantation report 2008. J Heart LungTransplant 2008; 27: 957-69.
30. de Perrot M, Chaparro C, McRae K et al. Twenty year experience of lung transplantation at a single center: Influence of recipient diagnosis on long-term survival. J Thorac Cardiovasc Surg 2004; 127: 1493-501.
31. Christie JD, Edwards LB, Aurora P et al. The Registry of the International Society for Heart and Lung Transplantation: Twenty-sixth Official Adult Lung and Heart-Lung Transplantation Report-2009. J Heart Lung Transplant 2009; 28: 1031-49.
32. Kotloff RM. Does lung transplantation confer a survival benefit? Curr Opin Organ Transplant 2009; 14: 499-503. 33. Lahzami S, Aubert JD. Lung transplantation for COPD - evidence-based? Swiss Med Wkly 2009; 139: 4-8.
34. Lawrence EC. Lung transplantation for COPD: one lung, two lungs, or none? Lancet 2008; 371: 702-3.
35. Marulli G, Rea F. Lung transplantation for emphysema. Transplant Proc2008; 40: 2006-9.
36. Groen H, van der Bij W, Koeter GH, TenVergert EM. Costeffectiveness of lung transplantation in relation to type of end-stage pulmonary disease. Am JTransplant 2004; 4: 1155-62.
37. Thabut G, Ravaud P, Christie JD et al. Determinants of the survival benefit of lung transplantation in patients with chronic obstructive pulmonary disease. Am J Respir Crit Care Med 2008; 177: 1156-63.
38. De Meester J, Smits JM, Persijn GG, Haverich A. Listing for lung transplantation: life expectancy and transplant effect, stratified by type of end-stage lung disease, the Eurotransplant experience. J Heart Lung Transplant 2001; 20: 518-24.
39. Tanash HA, Riise GC, Hansson L, Nilsson PM, Piitulainen E. Survival benefit of lung transplantation in individuals with severe alpha (1)-antitrypsin deficiency (PiZZ) and emphysema. J Heart Lung Transplant 2011; 30: 1342-7.